Take a Tour!
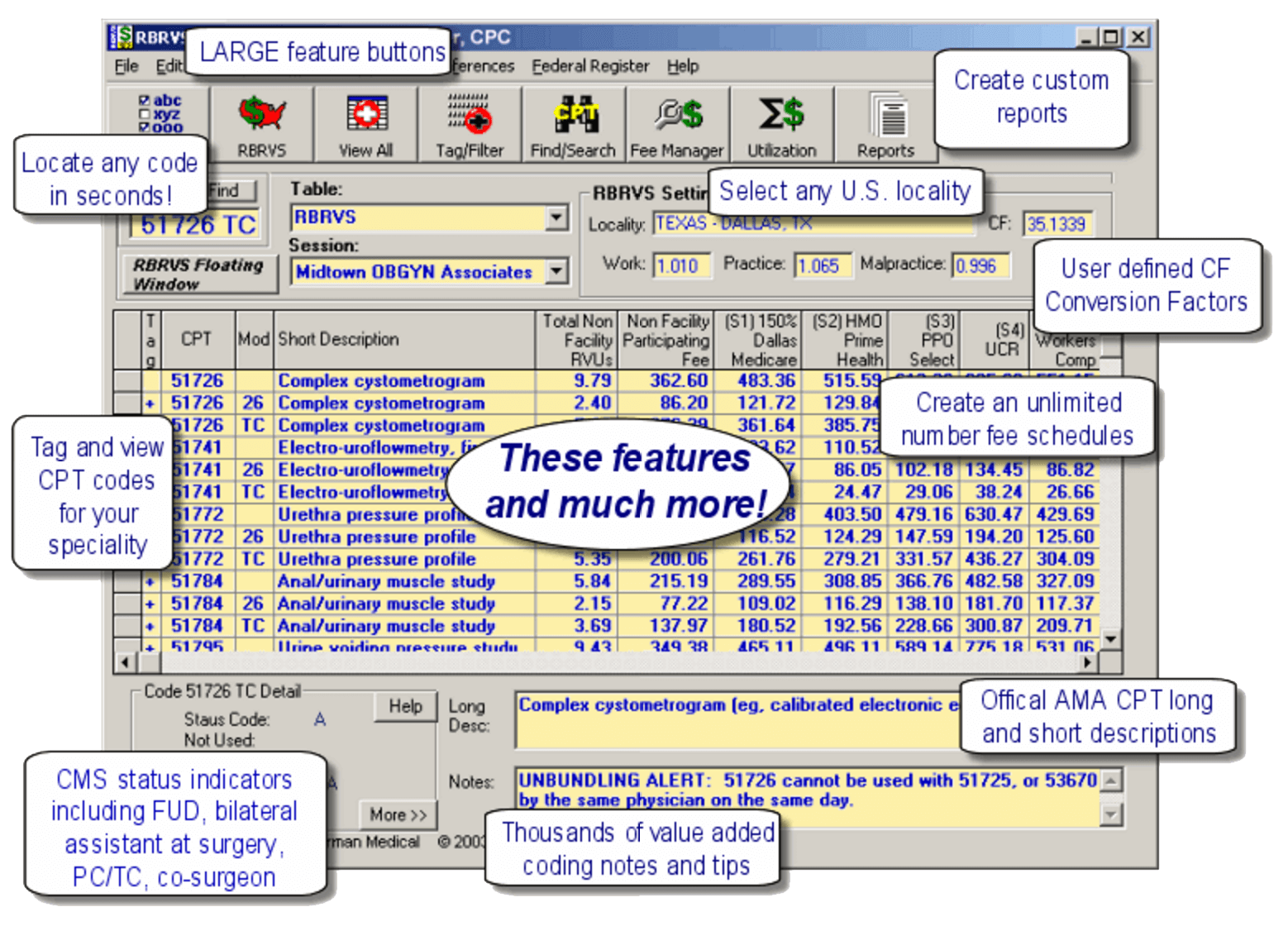
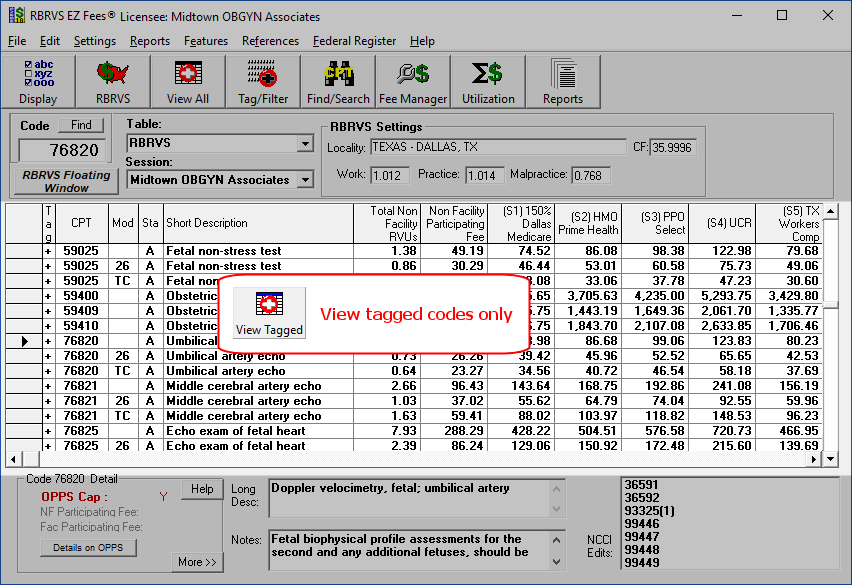
The View Tagged button allows for viewing tagged codes only. Tagging allows you to select only those code you are interested in viewing or printing. Tagged codes have a “+” sign on the main screen.
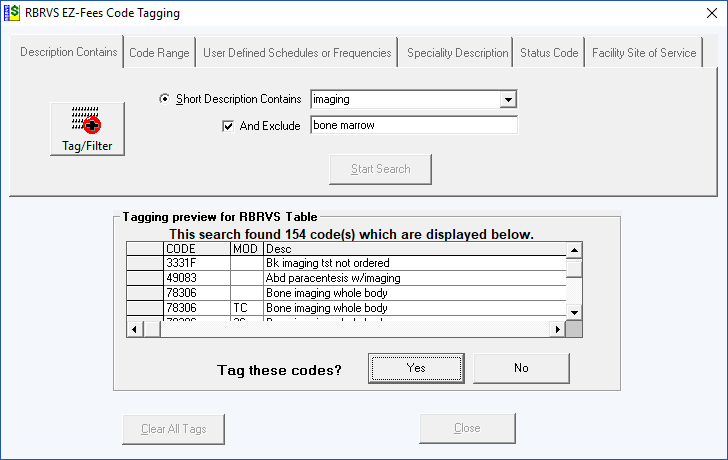
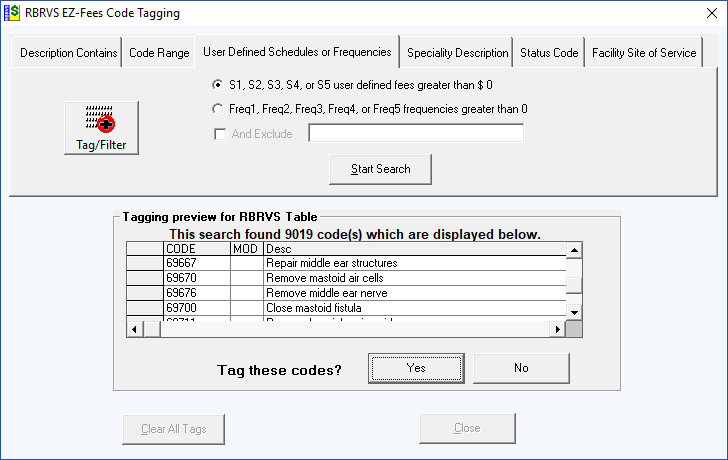
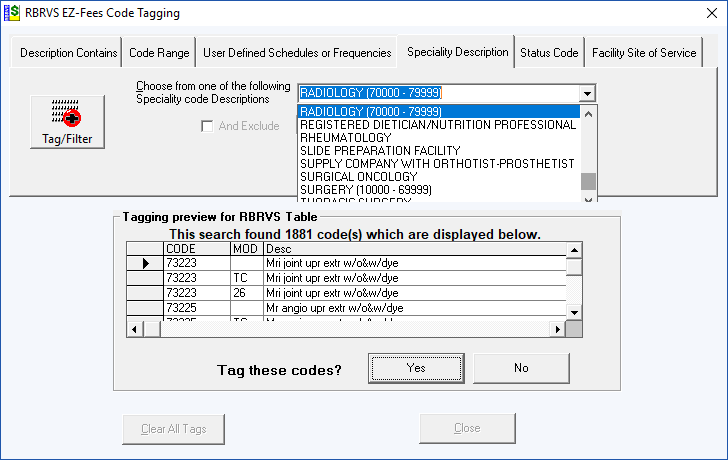
The Tag/Filter button allows for tagging (book marking) procedure codes based on Description, Code Range, Fee or Frequency Values, Medical Specialty and Code Status. Tagged codes can then be selected to be viewed only on the main screen and printed. Tagging is cumulative – meaning you can make several passes to tag additional codes that meet different search criteria. You can clear, save and load a tag list. RBRVS EZFees contains several tagging methods.
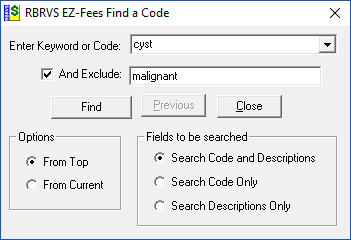
The Find / Search button searches for any keyword or code with several options to assist in locating difficult to find codes. The dropdown list hold the last 10 keywords.
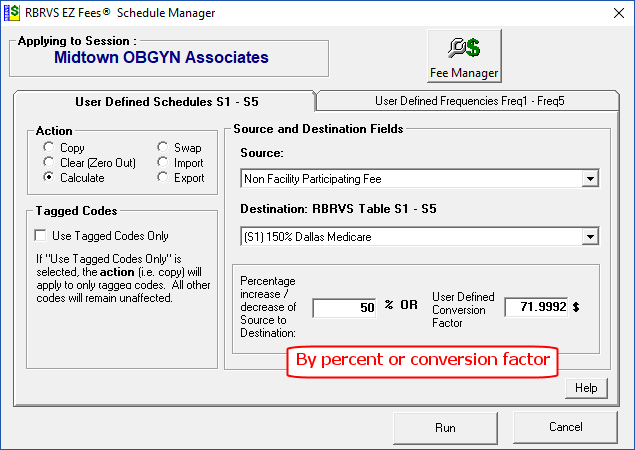
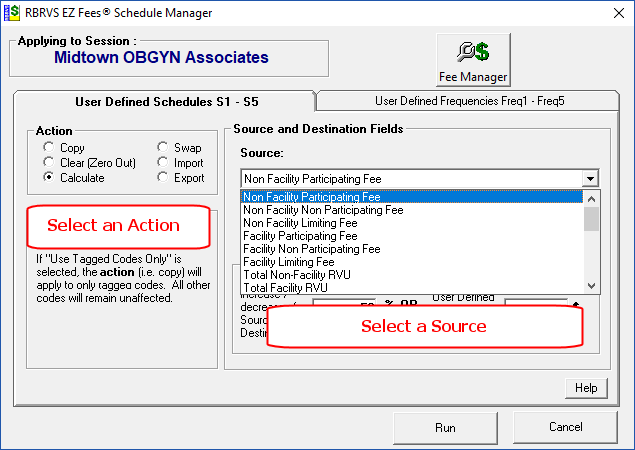
The Fee Manager button allows the user to create and modify fee schedules. In this example, the user is creating a fee schedule called Dallas Medicare that is above the Non participating Medicare Fee Schedule for Dallas, Texas.
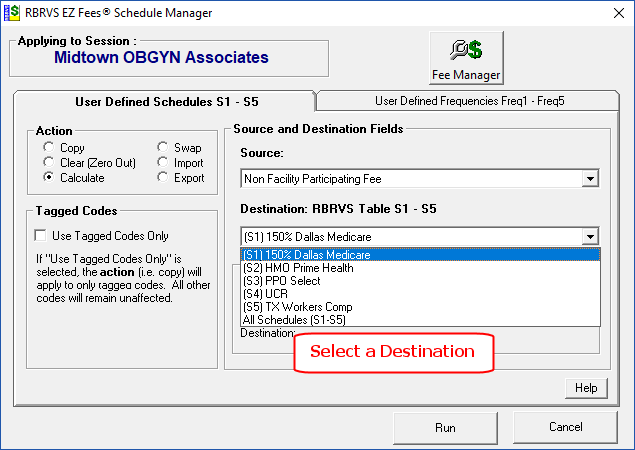
The “Source” can be any of the 6 Medicare Fee Schedules or any of the 5 User Defined Fee Schedules.
The “Destination” is any of the 5 User defined Fee Schedules
There are two tabs in the Schedule Manager: Fee Schedules and Frequency Schedules. You can perform the same operations on up to 5 User Define Frequency Schedules.
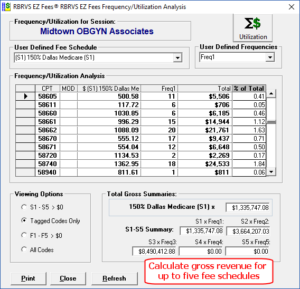
The Utilization / Frequency feature shows procedure code, selected user defined fee and frequency schedule and total (user defined fee time frequency and percent of total schedule).
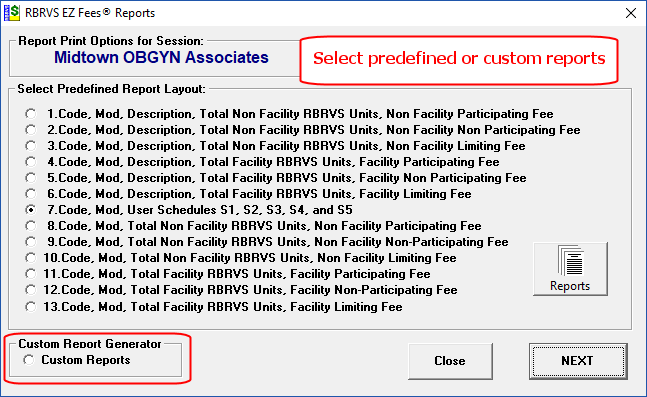
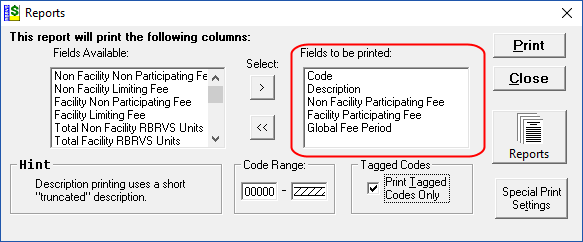
The Reports button brings up 13 common pre-defined report layouts.For custom reports select the “Custom Reports” option. Custom Reports allows for user defined fields. The “Print Tagged Codes Only” check box is an excellent way to print only those codes you wish to include in your report.
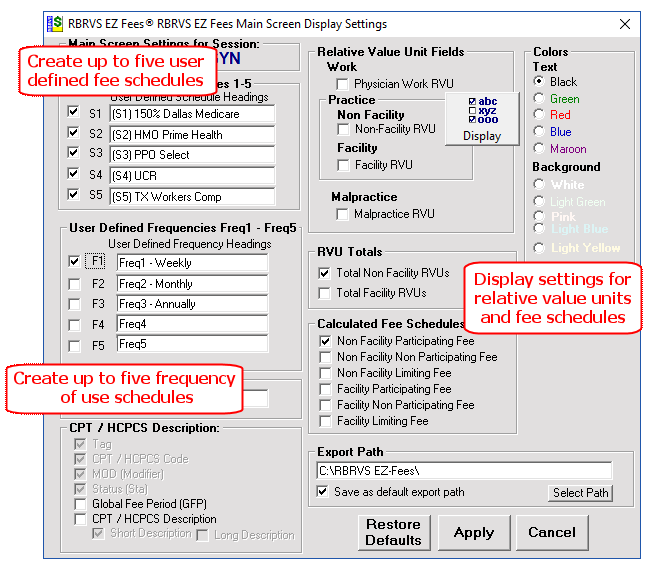
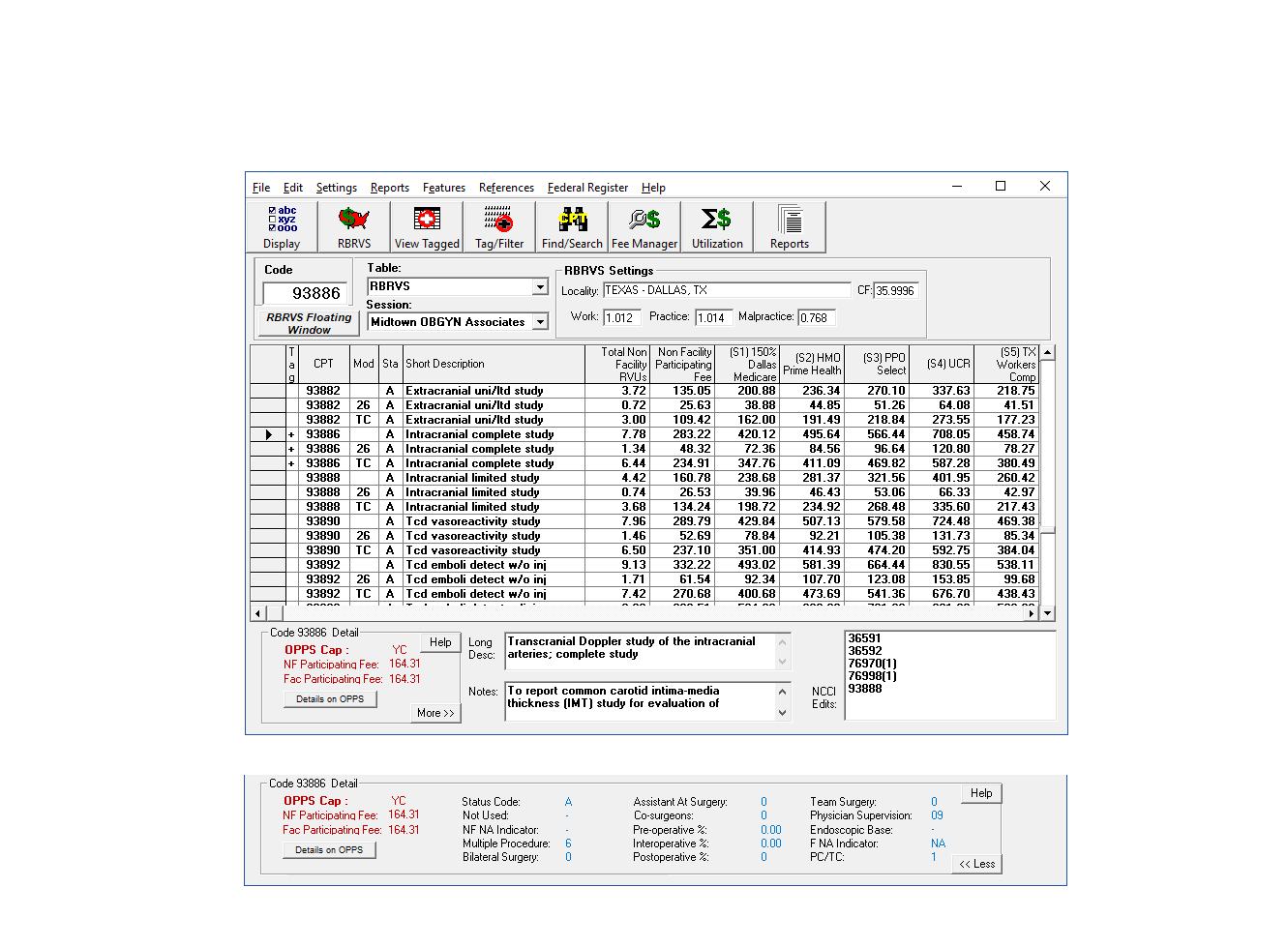
There are over 12,000 CPT and HCPCS codes in the RBRVS table. The RBRVS table columns can be customized for your viewing specifications by selecting the Display button.
The more button on the Code Detail displays every CMS Status indicator and with a convenient Help button for definitions. See the Tables section for more information and definitions.
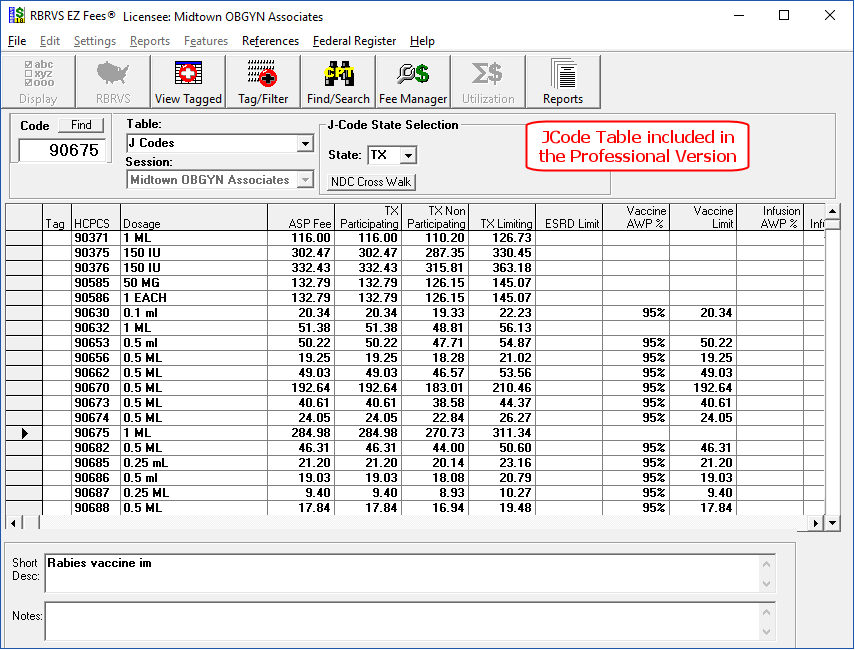
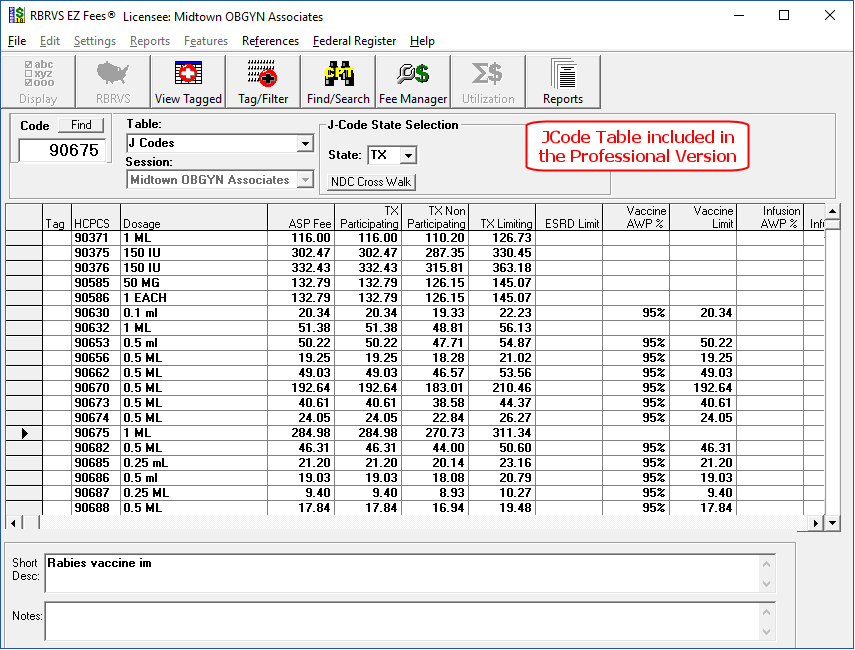
There are over 600 CPT HCPCS codes in the J Code table. The Help button provides additional information on J Code pricing.
There are over 1100 lab CPT codes in the LAB Table. The Help button provides additional information on LAB pricing.
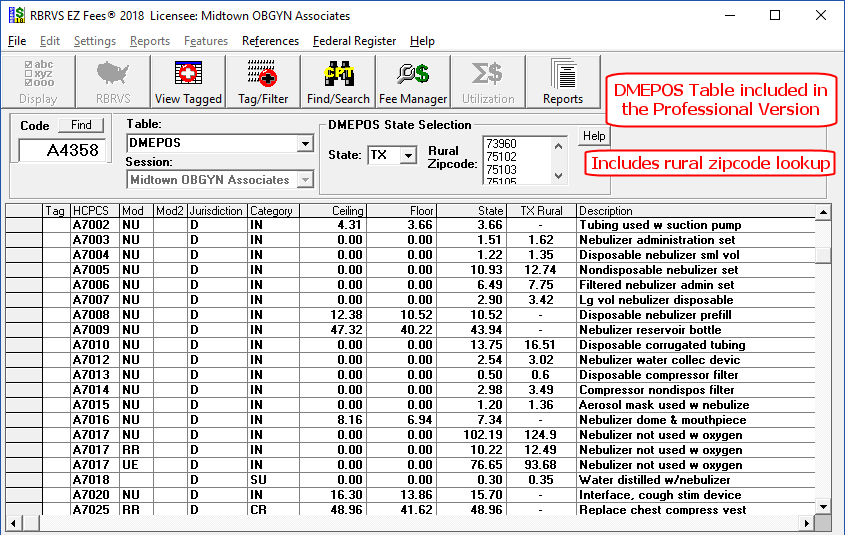
There are over 2600 HCPCS codes in the DMEPOS Table. The Help button provides additional information on DMEPOS pricing.
Code Detail (Status Indicators)
The code detail section on the main screen provides Medicare Billing information per current lookup CPT code. The following is a summary of these fields:
Status Code
Indicates whether the code is in the fee schedule and whether it is separately payable if the service is covered. Only RVUs associated with status codes of “A”, “R”, or “T”, are used for Medicare payment.
A =Active Code. These codes are paid separately under the physician fee schedule, if covered. There will be RVUs for codes with this status. The presence of an “A” indicator does not mean that Medicare has made a national coverage determination regarding the service; carriers remain responsible for coverage decisions in the absence of a national Medicare policy.
B =Bundled Code. Payment for covered services are always bundled into payment for other services not specified. There will be no RVUs or payment amount for these codes, and no separate payment is made. When these services are covered, payment for them is subsumed by the payment for the services to which they are incident. (An example is a telephone call from a hospital nurse regarding care of a patient).
C =Carriers price the code. Carriers will establish RVUs and payment amounts for these services, generally on an individual case basis following review of documentation such as an operative report.
D =Deleted Codes. These codes are deleted effective with the beginning of the applicable year.
E =Excluded from Physician Fee Schedule by regulation. These codes are for items and/or services that CMS chose to exclude from the fee schedule payment by regulation. No RVUS or payment amounts are shown and no payment may be made under the fee schedule for these codes. Payment for them, when covered, generally continues under reasonable charge procedures.
F =Deleted/Discontinued Codes. (Code not subject to a 90 day grace period).
G =Not valid for Medicare purposes. Medicare uses another code for reporting of, and payment for, these services. (Code subject to a 90 day grace period.)
g = Gap Code
H =Deleted Modifier. This code had an associated TC and/or 26 modifier in the previous year. For the current year, the TC or 26 component shown for the code has been deleted, and the deleted component is shown with a status code of “H”.
I = Not valid for Medicare purposes. Medicare uses another code for reporting of, and payment for, these services. (Code NOT subject to a 90 day grace period.)
N =Noncovered Services. These services are not covered by Medicare.
P =Bundled/Excluded Codes. There are no RVUs and no payment amounts for these services. No separate payment should be made for them under the fee schedule.
–If the item or service is covered as incident to a physician service and is provided on the same day as a physician service, payment for it is bundled into the payment for the physician service to which it is incident. (An example is an elastic bandage furnished by a physician incident to physician service.)
–If the item or service is covered as other than incident to a physician service, it is excluded from the fee schedule (i.e., colostomy supplies) and should be paid under the other payment provision of the Act.
R =Restricted Coverage. Special coverage instructions apply. If covered, the service is carrier priced. (NOTE: The majority of codes to which this indicator will be assigned are the alpha-numeric dental codes, which begin with “D”. We are assigning the indicator to a limited number of CPT codes which represent services that are covered only in unusual circumstances.)
T =Injections. There are RVUS and payment amounts for these services, but they are only paid if there are no other services payable under the physician fee schedule billed on the same date by the same provider. If any other services payable under the physician fee schedule are billed on the same date by the same provider, these services are bundled into the physician services for which payment is made. (NOTE: This is a change from the previous definition, which states that injection services are bundled into any other services billed on the same date.)
X =Statutory Exclusion. These codes represent an item or service that is not in the statutory definition of “physician services” for fee schedule payment purposes. No RVUS or payment amounts are shown for these codes, and no payment may be made under the physician fee schedule. (Examples are ambulance services and clinical diagnostic laboratory services.)
Not Used for Medicare Payment Purposes Indicator
An + in this field Indicates that the relative value units are not used for Medicare payment purposes.
Non Facility NA Indicator
An NA in this field indicates that this procedure is rarely or never performed in the non-facility setting.
Facility NA Indicator
An NA in this field indicates that this procedure is rarely or never performed in the facility setting.
PC/TC Indicator
0 = Physician Service Codes–Identifies codes that describe physician services. Examples include visits, consultations, and surgical procedures. The concept of PC/TC does not apply since physician services cannot be split into professional and technical components. Modifiers 26 and TC cannot be used with these codes. The RVUS include values for physician work, practice expense and malpractice expense. There are some codes with no work RVUs.
1 = Diagnostic Tests for Radiology Services–Identifies codes that describe diagnostic tests. Examples are pulmonary function tests or therapeutic radiology procedures, e.g., radiation therapy. These codes have both a professional and technical component. Modifiers 26 and TC can be used with these codes. The total RVUs for codes reported with a 26 modifier include values for physician work, practice expense, and malpractice expense. The total RVUs for codes reported with a TC modifier include values for practice expense and malpractice expense only. The total RVUs for codes reported without a modifier include values for physician work, practice expense, and malpractice expense.
2 = Professional Component Only Codes–This indicator identifies stand-alone codes that describe the physician work portion of selected diagnostic tests for which there is an associated code that describes the technical component of the diagnostic test only and another associated code that describes the global test. An example of a professional component only code is 93010–Electrocardiogram; Interpretation and Report. Modifiers 26 and TC cannot be used with these codes. The total RVUs for professional component only codes include values for physician work, practice expense, and malpractice expense.
3 = Technical Component Only Codes–This indicator identifies stand- alone codes that describe the technical component (i.e., staff and equipment costs) of selected diagnostic tests for which there is an associated code that describes the professional component of the diagnostic test only. An example of a technical component only code is 93005–Electrocardiogram; Tracing Only, without interpretation and report. It also identifies codes that are covered only as diagnostic tests and therefore do not have a related professional code. Modifiers 26 and TC cannot be used with these codes. The total RVUs for technical component only codes include values for practice expense and malpractice expense only.
4 = Global Test Only Codes–This indicator identifies stand-alone codes that describe selected diagnostic tests for which there are associated codes that describe (a) the professional component of the test only, and (b) the technical component of the test only. Modifiers 26 and TC cannot be used with these codes. The total RVUs for global procedure only codes include values for physician work, practice expense, and malpractice expense. The total RVUs for global procedure only codes equals the sum of the total RVUs for the professional and technical components only codes combined.
5 = Incident To Codes–This indicator identifies codes that describe services covered incident to a physician’s service when they are provided by auxiliary personnel employed by the physician and working under his or her direct personal supervision. Payment may not be made by carriers for these services when they are provided to hospital inpatients or patients in a hospital outpatient department. Modifiers 26 and TC cannot be used with these codes.
6 = Laboratory Physician Interpretation Codes–This indicator identifies clinical laboratory codes for which separate payment for interpretations by laboratory physicians may be made. Actual performance of the tests is paid for under the lab fee schedule. Modifier TC cannot be used with these codes. The total RVUs for laboratory physician interpretation codes include values for physician work, practice expense, and malpractice expense.
7 = Physical therapy service, for which payment may not be made–Payment may not be made if the service is provided to either a patient in a hospital outpatient department or to an inpatient of the hospital by an independently practicing physical or occupational therapist.
8 = Physician interpretation codes: This indicator identifies the professional component of clinical laboratory codes for which separate payment may be made only if the physician interprets an abnormal smear for hospital inpatient. This applies to codes 88141, 85060 and P3001-26. No TC billing is recognized because payment for the underlying clinical laboratory test is made to the hospital, generally through the PPS rate.
No payment is recognized for codes 88141, 85060 or P3001-26 furnished to hospital outpatients or non-hospital patients. The physician interpretation is paid through the clinical laboratory fee schedule payment for the clinical laboratory test.
9 = Not Applicable–Concept of a professional/technical component does not apply.
Preoperative Percentage
Percentage for preoperative portion of global package.
Intraoperative Percentage
Percentage for intraoperative portion of global package, including postoperative work in the hospital.
Postoperative Percentage
Percentage for postoperative portion of global package that is provided in the office after discharge from the hospital.
Multiple Procedure (Modifier 51)
Indicates applicable payment adjustment rule for multiple procedures:
0= No payment adjustment rules for multiple procedures apply. If procedure is reported on the same day as another procedure, base the payment on the lower of (a) the actual charge, or (b) the fee schedule amount for the procedure.
1= Standard payment adjustment rules in effect before January 1, 1995 for multiple procedures apply. In the 1995 file, this indicator only applies to codes with a status code of “D”. If procedure is reported on the same day as another procedure that has an indicator of 1, 2, or 3, rank the procedures by fee schedule amount and apply the appropriate reduction to this code 100, 50, 25, 25, 25, and by report). Base the payment on the lower of (a) the actual charge, or (b) the fee schedule amount reduced by the appropriate percentage.
2= Standard payment adjustment rules for multiple procedures apply. If procedure is reported on the same day as another procedure with an indicator of 1, 2, or 3, rank the procedures by fee schedule amount and apply the appropriate reduction to this code (100, 50, 50, 50, 50 and by report). Base the payment on the lower of (a) the actual charge, or (b) the fee schedule amount reduced by the appropriate percentage.
3= Special rules for multiple endoscopic procedures apply if procedure is billed with another endoscopy in the same family (i.e., another endoscopy that has the same base procedure). The base procedure for each code with this indicator is identified in the Endobase field of this file. Apply the multiple endoscopy rules to a family before ranking the family with the other procedures performed on the same day (for example, if multiple endoscopies in the same family are reported on the same day as endoscopies in another family or on the same day as a non-endoscopic procedure). If an endoscopic procedure is reported with only its base procedure, do not pay separately for the base procedure. Payment for the base procedure is included in the payment for the other endoscopy.
9= Concept does not apply.
Bilateral Surgery(Modifier 50)
Indicates services subject to payment adjustment.
0= 150 payment adjustment for bilateral procedures does not apply. If procedure is reported with modifier -50 or with modifiers RT and LT, base the payment for the two sides on the lower of: (a) the total actual charge for both sides or (b) 100 of the fee schedule amount for a single code. Example: The fee schedule amount for code XXXXX is $125. The physician reports code XXXXX-LT with an actual charge of $100 and XXXXX-RT with an actual charge of $100. Payment should be based on the fee schedule amount ($125) since it is lower than the total actual charges for the left and right sides ($200).
The bilateral adjustment is inappropriate for codes in this category (a) because of physiology or anatomy, or (b) because the code description specifically states that it is a unilateral procedure and there is an existing code for the bilateral procedure.
1= 150 payment adjustment for bilateral procedures applies. If the code is billed with the bilateral modifier or is reported twice on the same day by any other means (e.g., with RT and LT modifiers, or with a 2 in the units field), base the payment for these codes when reported as bilateral procedures on the lower of: (a) the total actual charge for both sides or (b) 150 of the fee schedule amount for a single code. If the code is reported as a bilateral procedure and is reported with other procedure codes on the same day, apply the bilateral adjustment before applying any multiple procedure rules.
2= 150 payment adjustment does not apply. RVUs are already based on the procedure being performed as a bilateral procedure. If the procedure is reported with modifier -50 or is reported twice on the same day by any other means (e.g., with RT and LT modifiers or with a 2 in the units field), base the payment for both sides on the lower of (a) the total actual charge by the physician for both sides, or (b) 100 of the fee schedule for a single code. Example: The fee schedule amount for code YYYYY is $125. The physician reports code YYYYY-LT with an actual charge of $100 and YYYYY-RT with an actual charge of $100. Payment should be based on the fee schedule amount ($125) since it is lower than the total actual charges for the left and right sides ($200).
The RVUs are based on a bilateral procedure because (a) the code descriptor specifically states that the procedure is bilateral, (b) the code descriptor states that the procedure may be performed either unilaterally or bilaterally, or (c) the procedure is usually performed as a bilateral procedure.
3= The usual payment adjustment for bilateral procedures does not apply. If the procedure is reported with modifier -50 or is reported for both sides on the same day by any other means (e.g., with RT and LT modifiers or with a 2 in the units field), base the payment for each side or organ or site of a paired organ on the lower of (a) the actual charge for each side or (b) 100 of the fee schedule amount for each side. If the procedure is reported as a bilateral procedure and with other procedure codes on the same day, determine the fee schedule amount for a bilateral procedure before applying any multiple procedure rules. Services in this category are generally radiology procedures or other diagnostic tests which are not subject to the special payment rules for other bilateral surgeries.
9= Concept does not apply.
Assistant at Surgery
Indicates services where an assistant at surgery is never paid for per Medicare Claims Manual.
0= Payment restriction for assistants at surgery applies to this procedure unless supporting documentation is submitted to establish medical necessity.
1= Statutory payment restriction for assistants at surgery applies to this procedure. Assistant at surgery may not be paid.
2= Payment restriction for assistants at surgery does not apply to this procedure. Assistant at surgery may be paid.
9= Concept does not apply.
Co-surgeons(Modifier 62)
Indicates services for which two surgeons, each in a different specialty, may be paid.
0= Co-surgeons not permitted for this procedure.
1= Co-surgeons could be paid, though supporting documentation is required to establish the medical necessity of two surgeons for the procedure.
2= Co-surgeons permitted and no documentation required if the two-specialty requirement is met.
9= Concept does not apply.
Team Surgery (Modifier 66)
Indicates services for which team surgeons may be paid.
0= Team surgeons not permitted for this procedure.
1= Team surgeons could be paid, though supporting documentation required to establish medical necessity of a team; pay by report.
2= Team surgeons permitted; pay by report.
9= Concept does not apply.
Physician Supervision
This field is for informational use only for of Diagnostic post payment review.
1 = Procedure must be performed under the general supervision of a physician.
2 = Procedure must be performed under the direct supervision of a physician.
3 = Procedure must be performed under the personal supervision of a physician.
4 = Physician supervision policy does not apply when procedure personally furnished by a qualified, independent psychologist or a clinical psychologist; otherwise must be performed under the general supervision of a physician.
5 = Physician supervision policy does not apply when procedure personally furnished by a qualified audiologist; otherwise must be performed under the general supervision of a physician.
6 = Procedure must be personally performed by a physician OR a physical therapist who is certified by the American Board of Physical Therapy Specialties as a qualified electrophysiologic clinical specialist AND is permitted to provide the service under State law.
7 = Procedure must be personally performed by a physical therapist who is certified by the American Board of Physical Therapy Specialties as a qualified electrophysiologic clinical specialist AND is permitted to provide the service under State law OR performed under the direct supervision of a physician.
8 = For future use.
9 = Concept does not apply.
P = Decision pending.
Billable Medical Supplies
Indicates services subject to special payment rules for supplies/administration.
0= Cannot be billed separately with this service.
1= Code in related procedure code field can be paid separately when billed with these procedures when service is performed in a physician’s office.
9= Concept does not apply.
Billable Medical Code
Related code referenced in Billable Medical Supplies (see above).
Endoscopic Base Code
Code which identifies an endoscopic base code for each code with a multiple surgery indicator of 3.
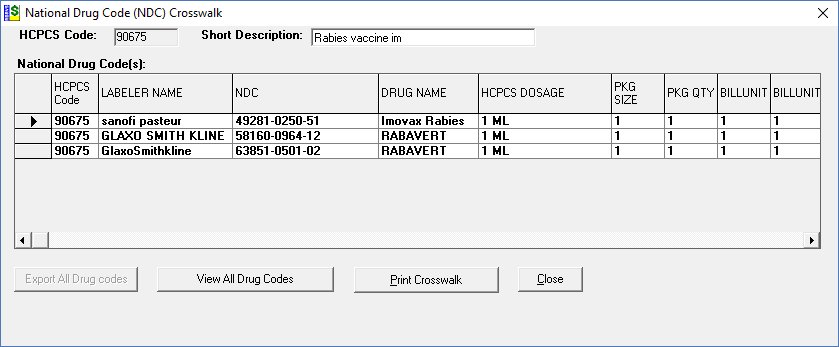
NDC Crosswalks are available by selecting the NDC Crosswalk button.
J Code Overview
Section 303(c) of the Medicare Modernization Act of 2003 (MMA) revised the payment methodology for Part B covered drugs that are not paid on a cost or prospective payment basis. In particular, section 303(c) of the MMA amended Title XVIII of the Act by adding section 1847A, which established a new average sales price (ASP) drug payment system. Beginning January 1, 2005, drugs and biologicals not paid on a cost or prospective payment basis will be paid based on the ASP methodology, and payment to the providers will be 106 percent of the ASP. There are exceptions to this general rule which are listed in the latest ASP quarterly change request (CR) document. The ASP methodology uses quarterly drug pricing data submitted to the CMS by drug manufacturers. CMS will supply contractors with the ASP drug pricing files for Medicare Part B drugs on a quarterly basis.
Par = Participating
Non Par = Non Participating = 95 of Par
Limiting = 115 of Non Par
ASP Drug Pricing Files and NDC-HCPCS Crosswalks Details
The J Code table above contains the payment amounts that will be used to pay for Part B covered drugs for the first quarter of 2006. Comparing the first quarter 2006 payment amounts with the previous quarters reveals that for the most part average drug prices in the market remain stable. Payment amounts across all drugs have decreased on average (weighted by Medicare expenditures) by less than 1 percent. For the top physician administered drugs, the payment amounts (weighted by Medicare expenditures) in aggregate changed little from last quarter. Preliminary 2005 data for the top physician administered drugs suggests that overall utilization of these drugs appears to have increased compared with 2004 levels.
For most of the higher volume drugs (29 out of the top 39), the payment amounts changed 2 percent or less, and for 23 of these codes the change is about 1 percent. Overall, the payment amounts for 23 of the top 39 drugs increased. Among the top drugs with a decrease, in general, there are a number of competitive market factors at work — multiple manufacturers, alternative therapies, new products, recent generic entrants, or market shifts to lower priced products.
Recent studies of Medicare payment rates for oncology drugs by the Department of Health and Human Services Office of Inspector General and the Medicare Payment Advisory Commission have found that physicians are generally able to acquire these drugs at prices below the Medicare reimbursement rate. CMS will continue to support groups representing Medicare Part B drug purchasers, especially small and rural purchasers, to help them identify the most favorable drug prices possible.
The payment amounts are 106 percent of the Average Sales Price (ASP) calculated from data submitted by drug manufacturers. The quarter to quarter price changes are the result of updated data from the manufacturers of these drugs.
Medicare Contractor Reporting Template for Medicare Part B Drugs – (Located in the Related Links section below)
As indicated in CR 4140, dated November 4, 2005, Medicare contractors shall use the Medicare Contractor Reporting Template for Part B drugs to report information on all Medicare Part B drugs not paid on a cost or prospective payment basis when payment limits are not listed in the quarterly drug pricing files, or in the OPPS Pricer. Contractors shall also use the template to report pricing information for the NOC drug billing codes. This information must be sent to CMS on a monthly basis to e-mail address: sec303aspdata@cms.hhs.gov.
LAB Table (Clinical Diagnostic Lab Fee Schedule CLAB)
The Clinical Lab fee schedule contains national limits and pricing amounts for each procedure code subject to the Clinical Lab fee schedule payment methodology.
HCPCS CODE
All current year active and deleted CPT and alpha-numeric codes subject to the Clinical Laboratory Fee Schedule.
MODIFIER
Where modifier is shown, QW denotes a CLIA waiver test.
NATIONAL LIMITATION AMOUNT
The National Limitation Amount is set at 74 of the 2003 median. The 62 National Limitation Amount can be computed using the following algorithm: (60 National Limitation Amount / .60) * .62
If the floor is applicable, then the National Limitation Amount is appropriately adjusted.
MEDIAN
Median of the 2003 60 Updated Base Fee Amounts from all Medicare Part B Carriers.
60 FLOOR
BBRA of 1999 requires a payment floor of $14.60 for all Pap Smears; the floor equals the 60 floor.
Notes:
(1) The 60 Pricing Amount is the lower of the National Limitation Amount or the Updated Base Fee Amount. If the floor is applicable, then the pricing amount is appropriately adjusted.
(2) The 62 Pricing Amount can be computed using the following algorithm: (60 Pricing Amount / .60) * .62) If the floor is applicable, then the pricing amount is appropriately adjusted.
STATES:
CARRIER 00510 (ALABAMA) 60 PRICING AMOUNT
CARRIER 00511 (GEORGIA) 60 PRICING AMOUNT
CARRIER 00512 (MISSISSIPPI) 60 PRICING AMOUNT
CARRIER 00520 (ARKANSAS) 60 PRICING AMOUNT
CARRIER 00521 (NEW MEXICO) 60 PRICING AMOUNT
CARRIER 00522 (OKLAHOMA) 60 PRICING AMOUNT
CARRIER 00523 (MISSOURI GENERAL AMERICAN) 60 PRICING AMOUNT
CARRIER 00528 (LOUISIANA) 60 PRICING AMOUNT
CARRIER 00590 (FLORIDA) 60 PRICING AMOUNT
CARRIER 00591 (CONNECTICUT) 60 PRICING AMOUNT
CARRIER 00630 (INDIANA) 60 PRICING AMOUNT
CARRIER 00650 (KANSAS) 60 PRICING AMOUNT
CARRIER 00655 (NEBRASKA) 60 PRICING AMOUNT
CARRIER 00660 (KENTUCKY) 60 PRICING AMOUNT
CARRIER 00740 (MISSOURI) 60 PRICING AMOUNT
CARRIER 00751 (MONTANA) 60 PRICING AMOUNT
CARRIER 00801 (WESTERN NEW YORK) 60 PRICING AMOUNT
CARRIER 00803 (EMPIRE NEW YORK) 60 PRICING AMOUNT
CARRIER 00805 (NEW JERSEY) 60 PRICING AMOUNT
CARRIER 00820/01 (NORTH DAKOTA) 60 PRICING AMOUNT
CARRIER 00820/02 (SOUTH DAKOTA) 60 PRICING AMOUNT
CARRIER 00824 (COLORADO) 60 PRICING AMOUNT
CARRIER 00825 (WYOMING) 60 PRICING AMOUNT
CARRIER 00826 (IOWA) 60 PRICING AMOUNT
CARRIER 00831 (ALASKA) 60 PRICING AMOUNT
CARRIER 00832 (ARIZONA) 60 PRICING AMOUNT
CARRIER 00833 (HAWAII) 60 PRICING AMOUNT
CARRIER 00834 (NEVADA) 60 PRICING AMOUNT
CARRIER 00835 (OREGON) 60 PRICING AMOUNT
CARRIER 00836 (WASHINGTON STATE) 60 PRICING AMOUNT
CARRIER 00865 (PENNSYLVANIA) 60 PRICING AMOUNT
CARRIER 00870 (RHODE ISLAND) 60 PRICING AMOUNT
CARRIER 00880 (SOUTH CAROLINA) 60 PRICING AMOUNT
CARRIER 00883 (OHIO) 60 PRICING AMOUNT
CARRIER 00884 (WEST VIRGINIA) 60 PRICING AMOUNT
CARRIER 00900 (TEXAS) 60 PRICING AMOUNT
CARRIER 00901 (MARYLAND) 60 PRICING AMOUNT
CARRIER 00902 (DELAWARE) 60 PRICING AMOUNT
CARRIER 00903 (DISTRICT OF COLUMBIA) 60 PRICING AMOUNT
CARRIER 00904 (VIRGINIA) 60 PRICING AMOUNT
CARRIER 00910 (UTAH) 60 PRICING AMOUNT
CARRIER 00951 (WISCONSIN) 60 PRICING AMOUNT
CARRIER 00952 (ILLINOIS) 60 PRICING AMOUNT
CARRIER 00953 (MICHIGAN) 60 PRICING AMOUNT
CARRIER 00954 (MINNESOTA) 60 PRICING AMOUNT
CARRIER 00973 (PUERTO RICO) 60 PRICING AMOUNT
CARRIER 05130 (IDAHO) 60 PRICING AMOUNT
CARRIER 05440 (TENNESSEE) 60 PRICING AMOUNT
CARRIER 05535 (NORTH CAROLINA) 60 PRICING AMOUNT
CARRIER 14330 (NEW YORK GHI) 60 PRICING AMOUNT
CARRIER 31140 (NORTHERN CALIFORNIA) 60 PRICING AMOUNT
CARRIER 31142 (MAINE) 60 PRICING AMOUNT
CARRIER 31143 (MASSACHUSETTS) 60 PRICING AMOUNT
CARRIER 31144 (NEW HAMPSHIRE) 60 PRICING AMOUNT
CARRIER 31145 (VERMONT) 60 PRICING AMOUNT
CARRIER 31146 (SOUTHERN CALIFORNIA OCCIDENTAL) 60 PRICING
Multi Schedule States
State Carriers
CA1 31146
CA2 31140
MO1 00740
MO2 00523
NY1 00801
NY2 00803
NY3 14330
To find a carrier’s locality description select the RBRVS table on the main screen, click on the large RBRVS button, select the change locality button and select a state.
GAP FILL INDICATOR
0–No Gap Filling Required
1–Carrier Needs to Gap Fill 60 and 62 Fee Schedules
Additional Notes on the LAB Table. In order to facilitate the distribution of pricing information for specimen collection services, this file contains pricing information for codes G0001, P9610, and P9612. CPT codes 80002 through 80019 for 1 through 19 non-specified automated multi-channel test and codes G0058-G0060 for 20-22 or more tests were deleted in 1998 and replaced by a new series of parallel HCFA payment codes (ATP02-ATP22). Instructions on the 2003 Clinical Diagnostic Laboratory Fee Schedule and Laboratory Services Paid Under Reasonable Charge Payment Methodology ere issued in Program Memorandum AB-02-163.
Durable Medical Equipment, Prosthetics/Orthotics, and Supplies Fee Schedule Table
The DMEPOS fee schedule contains fee schedule amounts, floors, and ceilings for each procedure code subject to the DMEPOS fee schedule payment methodology. Although these fee schedule amounts are contained in a single table, their calculations have been mandated by three separate payment methodologies: DME, prosthetic and orthotic, and surgical dressings. For further information on these payment methodologies and their policy histories, please refer to Background below.
Column Headings and Status Codes
HCPCS CODE
All current year active and deleted codes subject to DMEPOS floors and ceilings.
MODIFIER
NU–Purchased, New
RR–Rented
UE–Purchased, Used
KM-Replacement of Facial Prosthesis including new
impression/moulage
KN-Replacement of Facial Prosthesis using previous master mold
AU–Urological, ostomy or trach item
JURISDICTION
D–DMERC jurisdiction
L–Local Part B Carrier jurisdiction
J–Joint DMERC/Local Carrier jurisdiction
CATEGORY
IN–Inexpensive and Other Routinely Purchased Items
FS–Frequently Serviced Items
CR–Capped Rental Items
OX–Oxygen and Oxygen Equipment
OS–Ostomy, Tracheostomy & Urological Items
SD–Surgical Dressings
PO–Prosthetics & Orthotics
SU–Supplies
TE–Transcutaneous Electrical Nerve Stimulators
CEILING
Maximum fee schedule amount.
Please note that since E0607 is priced via national Inherent Reasonableness, it is not priced using floors and ceilings. For E0607, this field will be filled with zeros. Since pricing amounts for E1405 and E1406 were developed by summing pricing amounts from source codes, they are not subject to ceilings and floors.
FLOOR
Minimum fee schedule amount.
Please note that since E0607 is priced via national Inherent Reasonableness, it is not priced using floors and ceilings. For E0607, this field will be filled with zeros. Since pricing amounts for E1405 and E1406 were developed by summing pricing amounts from source codes, they are not subject to ceilings and floors.
Background:
Medicare payment for durable medical equipment (DME), prosthetics and orthotics (P&O), and surgical dressings is equal to 80 percent of the lower of either the actual charge for the item or the fee schedule amount calculated for the item, less any unmet deductible. The beneficiary is responsible for 20 percent of the lower of either the actual charge for the item or the fee schedule amount calculated for the item, plus any unmet deductible. The DME and P&O fee schedule payment methodology is mandated by section 4062 of the Omnibus Budget Reconciliation Act (OBRA) of 1987, which added section 1834(a) to the Social Security Act. OBRA of 1990 added a separate subsection, 1834(h), for P&O. The DME and P&O fee schedules were implemented on January 1, 1989 with the exception of the oxygen fee schedules, which were implemented on June 1, 1989. Section 13544 of OBRA of 1993, which added section 1834(i) to the Social Security Act, mandates a fee schedule for surgical dressings; the surgical dressing fee schedule was implemented on January 1, 1994. Section 4315 of the Balanced Budget Act of 1997, which added section 1842(s) to the Social Security Act, authorizes a fee schedule for parenteral and enteral nutrition (PEN); the PEN fee schedule was implemented on January 1, 2002.
DME Fee Schedule Payment Methodology
The DME fee schedules are calculated for the following DME payment classes:
INEXPENSIVE AND OTHER ROUTINELY PURCHASED ITEMS (Section 1834(a)(2))
These items have a purchase price of $150 or less, or are generally purchased 75 percent of the time or more, or are accessories used in conjunction with certain nebulizers, aspirators, and ventilators. If covered, these items can be purchased new or used and can be rented; however, total payments cannot exceed the purchase new fee for the item.
FREQUENTLY SERVICED ITEMS (Section 1834(a)(3))
These items require frequent and substantial servicing. Examples of such items are provided in section 1834(a)(3)(A). If covered, these items can be rented as long as they are medically necessary.
OXYGEN AND OXYGEN EQUIPMENT (Section 1834(a)(5))
Medicare payment for oxygen and oxygen equipment is made on a monthly basis. One bundled monthly payment amount is made for all covered stationary equipment, stationary and portable contents, and all accessories used in conjunction with the oxygen equipment. If the beneficiary owns her equipment and oxygen contents are covered, a monthly payment is made for oxygen contents only. An additional monthly payment may be made for those beneficiaries who require portable oxygen. If the beneficiary owns their portable equipment, then a monthly payment may be made for portable contents only.
OTHER COVERED ITEMS (OTHER THAN DME) (Section 1834(a)(6))
These are supplies that are necessary for the effective use of DME. Medicare payment is made for the purchase of these supplies, if covered.
CAPPED RENTAL ITEMS (Section 1834(a)(7))
These are items of DME which do not fall under any of the other DME payment categories. They are generally expensive items which have historically been routinely rented. In general, Medicare pays for the rental of these items, when covered, for a period of continuous use not to exceed 15 months. The beneficiary can decide to purchase the item in the tenth month of rental. In this case, Medicare rental payments are capped out@ at 13 months instead of 15 months. Power wheelchairs can be purchased in the first month of use.
The fee schedule amount is calculated based on 10 percent of the base year purchase price increased by the covered item update. This is the fee schedule amount for months 1 thru 3. Beginning with the fourth month, the fee schedule amount is equal to 75 percent of the fee schedule amount paid in the first three rental months. The purchase fee schedule amount for power wheelchairs is equal to the rental fee (for months 1 thru 3) multiplied by ten.
Fee schedule amounts are not calculated for customized DME:
CERTAIN CUSTOMIZED ITEMS (Section 1834(a)(4))
If covered, Medicare payment is made in a lump-sum amount for the purchase of the item; this payment amount is based on the carrier’s individual consideration for that item.
National Ceiling And Floor Limits for DME and Surgical Dressings
The fee schedule amounts for DME and surgical dressings are calculated on a statewide basis and are limited by national ceilings and floors. The fee schedule ceiling is equal to the median or mid-point of the statewide fee schedule amounts. The fee schedule floor is equal to 85 percent of the median of the statewide fee schedule amounts.
Covered Item Updates for DME and Surgical Dressings
The fee schedules for DME and surgical dressings are updated annually by a covered item update established through legislation. The covered item updates for 1990 through 2002 are:
1989 Initial Year of Fee Schedules
1990 0.0 percent
1991 3.7 percent
1992 3.7 percent
1993 3.1 percent
1994 3.0 percent
1995 2.5 percent
1996 3.0 percent
1997 2.8 percent
1998 0.0 percent
1999 0.0 percent
2000 0.0 percent
2001 3.7 percent (does not apply to oxygen and oxygen equipment or surgical dressings which received a 0.0 percent update for 2001)
2002 0.0 percent
2003 1.1 percent (does not apply to oxygen and oxygen equipment which received a 0.0 percent update for 2003)
2004 2.1 percent (does not apply to oxygen and oxygen equipment which received a 0.0 percent update for 2004)
P&O Fee Schedule Payment Methodology
Regional purchase (new) fee schedule amounts are calculated for P&O (section 1834(h)). The P&O payment class includes: ostomy, tracheostomy, and urological supplies; orthotics; prosthetics; prosthetic devices; and certain vision services. The regional fees are equal to the weighted average of the statewide fees in each HCFA Region.
* Per OBRA of 1993, effective January 1, 1994, the purchase (new) fee schedule amounts for ostomy, tracheostomy, and urological supplies are calculated using the same methodology as the purchase (new) fee schedule amounts for inexpensive or routinely purchased items of DME. As a result, these items are not subject to regional fee schedules. A fee schedule ceiling and floor, based on the median and 85 percent of the median, respectively, of the local fee schedule amounts are calculated for each item. The fee schedule amounts for these items are updated by the DME/surgical dressing covered item updates.
National Ceiling And Floor Limits for P&O
The P&O regional fee schedule amounts are limited by a ceiling (120{6ba4b1425649820a8750bcb7cfbb72a6d42a1a2610d1c3bb7116dfaa116e496e} of the average of the regional statewide fees) and a floor (90{6ba4b1425649820a8750bcb7cfbb72a6d42a1a2610d1c3bb7116dfaa116e496e} of the average of the regional statewide fees).
Covered Item Updates for P&O
The fee schedules for P&O are updated annually by a covered item update established through legislation. The covered item updates for 1990 through 2004 are:
1989 Initial Year of Fee Schedules
1990 0.0 percent
1991 0.0 percent
1992 4.7 percent
1993 3.1 percent
1994 0.0 percent
1995 0.0 percent
1996 3.0 percent
1997 2.8 percent
1998 1.0 percent
1999 1.0 percent
1999 1.0 percent
2000 1.0 percent
2001 3.7 percent
2002 1.0 percent
2003 1.1 percent
2004 2.1 Percent
PEN Fee Schedule Payment Methodology
The payment methodology for PEN changed effective January 1, 2002. Section 4315 of the Balanced Budget Act of 1997, which added section 1842(s) to the Social Security Act, authorizes a fee schedule for PEN. This fee schedule is a national fee schedule (i.e., no variation from state to state).
Covered Item Updates for PEN
2002 Initial Year
2003 1.1 percent
2004 2.1 percent
STATES:
ALABAMA FEE SCHEDULE AMOUNT
ARKANSAS FEE SCHEDULE AMOUNT
ARIZONA FEE SCHEDULE AMOUNT
CALIFORNIA FEE SCHEDULE AMOUNT
COLORADO FEE SCHEDULE AMOUNT
CONNECTICUT FEE SCHEDULE AMOUNT
DISTRICT OF COLUMBIA FEE SCHEDULE AMOUNT
DELAWARE FEE SCHEDULE AMOUNT
FLORIDA FEE SCHEDULE AMOUNT
GEORGIA FEE SCHEDULE AMOUNT
IOWA FEE SCHEDULE AMOUNT
IDAHO FEE SCHEDULE AMOUNT
ILLINOIS FEE SCHEDULE AMOUNT
INDIANA FEE SCHEDULE AMOUNT
KANSAS FEE SCHEDULE AMOUNT
KENTUCKY FEE SCHEDULE AMOUNT
LOUISIANA FEE SCHEDULE AMOUNT
MASSACHUSETTS FEE SCHEDULE AMOUNT
MARYLAND FEE SCHEDULE AMOUNT
MAINE FEE SCHEDULE AMOUNT
MICHIGAN FEE SCHEDULE AMOUNT
MINNESOTA FEE SCHEDULE AMOUNT
MISSOURI FEE SCHEDULE AMOUNT
MISSISSIPPI FEE SCHEDULE AMOUNT
MONTANA FEE SCHEDULE AMOUNT
NORTH CAROLINA FEE SCHEDULE AMOUNT
NORTH DAKOTA FEE SCHEDULE AMOUNT
NEBRASKA FEE SCHEDULE AMOUNT
NEW HAMPSHIRE FEE SCHEDULE AMOUNT
NEW JERSEY FEE SCHEDULE AMOUNT
NEW MEXICO FEE SCHEDULE AMOUNT
NEVADA FEE SCHEDULE AMOUNT
NEW YORK FEE SCHEDULE AMOUNT
OHIO FEE SCHEDULE AMOUNT
OKLAHOMA FEE SCHEDULE AMOUNT
OREGON FEE SCHEDULE AMOUNT
PENNSYLVANIA FEE SCHEDULE AMOUNT
RHODE ISLAND FEE SCHEDULE AMOUNT
SOUTH CAROLINA FEE SCHEDULE AMOUNT
SOUTH DAKOTA FEE SCHEDULE AMOUNT
TENNESSEE FEE SCHEDULE AMOUNT
TEXAS FEE SCHEDULE AMOUNT
UTAH FEE SCHEDULE AMOUNT
VIRGINIA FEE SCHEDULE AMOUNT
VERMONT FEE SCHEDULE AMOUNT
WASHINGTON FEE SCHEDULE AMOUNT
WISCONSIN FEE SCHEDULE AMOUNT
WEST VIRGINIA FEE SCHEDULE AMOUNT
WYOMING FEE SCHEDULE AMOUNT
ALASKA FEE SCHEDULE AMOUNT
Fee schedule amounts for non-continental areas are not subject to the ceilings and floors.
HAWAII FEE SCHEDULE AMOUNT
Fee schedule amounts for non-continental areas are not subject to the ceilings and floors.
PUERTO RICO FEE SCHEDULE AMT
Fee schedule amounts for non-continental areas are not subject to the ceilings and floors.
VIRGIN ISLANDS FEE SCHEDULE AMT
Fee schedule amounts for non-continental areas are not subject to the ceilings and floors.
There are over 2400 ASC (Ambulatory Surgical Center) codes in the ASC Table.
The Help button provides additional information on ASC pricing.
2004 National ASC Payment Rates
ASC payment group rates effective October 1, 2003 are as follows:
Group 1 – $340
Group 2 – $455
Group 3 – $520
Group 4 – $643
Group 5 – $731
Group 6 – $840 ($690 + $150 for intraocular lenses (IOLs));
Group 7 – $1015
Group 8 – $989 ($839 + $150 for IOLs).
Group 9 – $1366
The $150 payment allowance in groups 6 and 8 is for intraocular lenses.
The formula for creating ASC payment rates is as follows:
Payment group 1,2,3,4,5,7,9
(National ASC Payment Rate x .3445 (standardized labor related portion) x CMS wage index) +
(National ASC Payment Rate x .6555 (standardized non labor related portion))
Payment group 6 & 8
((National ASC Payment Rate – $150 (IOL Allowance))x .3445 (standardized labor related portion) x CMS wage index) +
((National ASC Payment Rate – $150 (IOL Allowance)) x .6555 (standardized non labor related portion)+
$150 (IOL Allowance)
Tutorial
The following is an tutorial is for providers/suppliers furnishing services/supplies to a Medicare carrier. This material is intended to complement and not replace Medicare program requirements as set forth in statute, regulations and manual instructions. It is the responsibility of each provider/supplier submitting claims to a Medicare carrier to familiarize themselves with Medicare coverage requirements.
Ambulatory Surgical Centers (ASCs) Tutorial on Billing
An ASC is a distinct entity which operates exclusively to provide outpatient surgical services to patients by entering into an agreement with the Health Care Financing Administration (CMS). ASCs must be state licensed and Medicare certified. ASCs must also enter into a written agreement with CMS to accept assignment on Medicare claims. Any hospital, clinic, physician or physician group wishing to participate and establish a Medicare approved ASC should contact the state agency listed below:
An ASC may be either independent (i.e., not a part of any other facility) or hospital affiliated. Hospital affiliated ASCs are those operated by hospitals under common ownership, licensure or control. To be covered as an ASC operated by a hospital, a facility must meet the following requirements:
· Elect to participate in the Medicare Part B program as an ASC and continue as such unless CMS determines there is good cause to do otherwise. (The ASC may not opt to change at will to bill as an outpatient area of that hospital for purposes of reimbursement advantage.)
· Be a separate identifiable entity. This means it must be physically, administratively, and financially independent and distinct from other hospital operations. The hospital affiliated ASC must be set up as a non-reimbursable cost center to the hospital. (Under this restriction, ordinary hospital outpatient departments providing ambulatory surgery services are not eligible to receive reimbursement from the Part B Carrier.)
· Meet all requirements for health and safety standards, and agree to the assignment, coverage and reimbursement rules applied to an independent ASC. These requirements will be specifically outlined during the state licensure and CMS approval proceedings. Licensure and CMS certification must precede Medicare Part B billing.
Note: As an Ambulatory Surgical Center, assignment is mandatory for ASC facility services but Medicare participation is voluntary.
Coverage
Covered ASC facility services are defined as those furnished by an ASC in connection with a covered surgical procedure which are otherwise covered if furnished on an inpatient or outpatient basis in a hospital in connection with that procedure. The facility payment rate includes only the covered ASC facility services.
When an ASC is assigned a provider number for billing purposes, a list of eligible ASC procedure codes will be provided. This list of covered procedures merely indicates procedures that are covered and reimbursable if performed in the ASC setting. It does not require such procedures to be performed in such settings, nor is any out-of-the-ordinary justification or special review required if listed procedures are performed on a hospital inpatient basis. The choice of operating site remains a matter for the professional judgment of the patient’s physician. Also, all the general coverage rules regarding the medical necessity of a given procedure are applicable to ASC services in the same manner as all other covered services.
c.1 Covered ASC Facility Services
Covered services which are included in the ASC facility rate are as follows:
· Nursing services, services of technical personnel, and other related services;
· Use of the ASC facilities by the patient;
· Drugs, biologicals, surgical dressings, supplies, splints, casts, appliances and equipment;
· Diagnostic or therapeutic items and services (including simple preoperative laboratory tests, e.g., urinalysis, blood hemoglobin or hematocrit);
· Administrative, record keeping and housekeeping items and services;
· Blood, blood plasma, platelets, etc., except for those to which the blood deductible applies;
· Materials for anesthesia; and
· Intraocular lenses (IOLs).
c.2 ASC Services Not Included in the ASC Facility Rate
In general, an item or service separately covered under Medicare is not considered to be a covered ASC facility service. Services which are not considered ASC facility services, such as physician services and prosthetic devices other than intraocular lenses (IOLs), may be covered and billable under other Medicare provisions. Certain items and services such as those listed below are otherwise covered under Medicare and may be provided in the ASC, but are not included in the ASC facility rate:
· Physician services;
· The sale, lease or rental of durable medical equipment (DME) to ASC patients for use in their homes;*
· Prosthetic devices, except intraocular lenses (IOLs) and prosthetic implants; *
· Ambulance services;
· Leg, arm, back and neck braces;*
· Artificial legs, arms and eyes; and*
· Independent laboratory services.
*Claims for these items must be billed to the appropriate Durable Medical Equipment Regional Carrier (DMERC).
Note: An ASC wishing to provide laboratory services directly must have its laboratory certified as an independent clinical laboratory for the services to be covered. The services must then be billed by the laboratory rather than the ASC. Or, if the ASC has no laboratory facilities of its own, the ASC should contract with a hospital laboratory or independent clinical laboratory to provide services for them. The laboratory should then, under provisions of the law, bill Medicare directly. In general, however, the necessary laboratory tests are done outside the ASC prior to scheduling of surgery, since the test results often determine whether the beneficiary should have the surgery done on an outpatient basis.
Reimbursement
ASC facility services are reimbursed based on prospectively determined rates. These rates are not based on Diagnostic Related Groups (DRGs) as are hospital services. Rather, they are based upon the classifications of procedures into different payment groups which are based on surgical procedure complexity. Rates by payment group are established by CMS.
CMS updates and publishes the rate setting methodology and establishes wage index (WI) tables to use for either urban or rural areas. Each ASC’s rates are calculated using CMS’s rate and wage indices according to the ASC’s location.
When changes are made to the WI or the facility base rate, rates will be recalculated as instructed by CMS and each ASC will be notified of its newly adjusted rate. The ASCs must ensure their charges are based upon the applicable rates in effect. That is, the billed amount should be equal to or greater than the applicable rate.
The carrier is required to pay these rates regardless of what is billed. Reporting less than the calculated facility group rate could cause problems with co-insurance collection.
Facility services are subject to the usual Medicare Part B 20 percent coinsurance and deductible requirements. Therefore, Medicare payment is 80 percent of the prospectively determined rate.
At no time should an ASC bill for anesthesiology, surgery or assistant at surgery services. The anesthesiologist, surgeon and assistant surgeon would be submitting separate claims for their professional reimbursement.
Exception: ASC employed CRNA services must be reported with the ASC’s provider number in block 33 or the EMC equivalent and the rendering CRNA’s number in block 24k or the EMC equivalent. Please refer to the claims completion chart for specifics on reporting.
Facility Reimbursement-Single Procedures
Approved surgical procedures are classified into eight payment groups for facility reimbursement purposes. All approved surgical procedures within the same payment group are reimbursed at a single rate. The standard, unadjusted* rates applicable to each of the payment groups for services are as follows:
*These are the ASC facility rates before the WI factor is applied. Each facility will receive its respective adjusted facility rates at the time they are approved.
Facility Reimbursement-Multiple Procedures
More than one surgical procedure may be performed in the same operative session. Special rules apply to this situation. When two or more procedures are performed, the ASC will be reimbursed at the full rate for the procedure classified in the highest payment group. Any other procedures performed during the same session are reimbursed at 50 of the procedure’s applicable group rate. If the procedures are within the same group, the ASC should be reimbursed for the full rate for one procedure and at 50 of the rate for the others.
Payment for eligible bilateral procedures will be reimbursed at 150 of the applicable rate. Procedures eligible for the bilateral payment adjustment are determined by CMS.
For example, if sinusotomy, maxillary (antrotomy); intranasal (procedure code 31020) is performed bilaterally in one operative session, report it as 31020 with a 50 modifier (bilateral procedure). Payment for bilateral procedures is calculated by multiplying the wage adjusted payment rate by 150 percent.
Reimbursement of Physicians’ Professional Services Provided In Connection With Covered ASC Surgical Procedures
Physician reimbursement for ASC approved procedures are subject to the coinsurance and deductible provisions. Payment is made at 80of the Medicare physician fee schedule. Fees for approved procedures in an ASC setting (place of service 24) are noted on the fee schedule as a facility fee.
The Medicare global fee policies which are applied to the procedure when performed by the physician on an inpatient hospital basis will be applied to physician services provided in an ASC.
Reporting Instructions for ASC Facility Services
· The ASC and the surgeon should both report the surgical procedure code which accurately reflects the service provided.
· Report the place of service as 24 (ambulatory surgical center).
· Report procedure code modifier SG (ambulatory surgical center facility services). Physicians should not report this modifier when billing for their professional service.
· Report referring physician name and UPIN.
Note: ASCs are required to report referring physician information for three procedures codes: 66983, 66984, 66985 and 66986.
Refer to claims completion chart for complete reporting information.
ASC Special Instructions
Molteno Valve
Effective with dates of service on or after March 1, 1991, Medicare Part B will separately reimburse ASCs for Molteno valves (L8612) implanted during covered glaucoma surgery. Molteno valves are considered prosthetic devices and are generally implanted into the eyes of patients with advanced glaucoma in order to preserve their sight. Report procedure code L8612 with a separate charge in addition to the charge for the facility service. Attach a complete legible copy of the actual invoice for the Molteno valve to the facility claim. The invoice must indicate the actual or acquisition cost of the Molteno valve, any handling or dispensing fees involved, and any discounts the ASC receives.
Report the individual acquisition cost. Refer to the claims completion chart.
Note: Invoices must be kept on file and available for carrier review in the provider’s office for verification purposes.
Corneal Tissue Acquisition
Reimbursement may be made for the “processing, preserving and transporting of corneal tissue” (code V2785), associated with keratoplasty procedures performed in an Ambulatory Surgical Center. Claims for code V2785 must be supported by an invoice from the supplying eye bank showing the actual cost incurred to acquire the corneal tissue. Code V2785 may be reimbursed as an add-on to the ASC facility fee.
Report the individual acquisition cost. Refer to the claims completion chart.
Note: Invoices must be kept on file and available for carrier review in the provider’s office for verification purposes.
Implantable Venous Access Portals
Payment may be made for implantable venous access portals (procedure code A4300) furnished by Medicare participating ASCs in conjunction with insertion of implantable venous access port, with or without subcutaneous reservoir (procedure code 36533).
Report procedure codes A4300 and A4301 with a separate charge in addition to the facility services.
Note: Invoices must be kept on file and available for carrier review in the provider’s office for verification purposes.
Prosthetic Implants
Medicare Part B will separately reimburse ASCs for prosthetics (procedure codes L8600 – L8690) implanted during the specified covered surgeries. Ambulatory Surgical Centers should use these codes when reporting implant procedure services. Report the specific prosthetic code and applicable charge on a separate line on the facility claim. All these prosthetics are related to procedures that are on the current ASC list.
Code Terminology
Integumentary System
L8600 Implantable breast prosthesis, silicone or equal
Head (skull, facial bones and temporomandibular joint)
L8610 Ocular
L8612 Aqueous shunt
L8613 Ossicula
L8614 Cochlear device/system
Upper extremity
L8630 Metacarpophalangeal joint
Lower extremity (joint: knee, ankle, toe)
L8641 Metatarsal joint
L8642 Hallux implant
Miscellaneous muscular-skeletal
L8658 Interphalangeal joint
Cardiovascular system
L8670 Vascular graft material, synthetic
Intraocular Lens (IOLs)
IOLs are “bundled” into facility payment groups 6 and 8. Do not bill separately for IOLs since the facility payment includes this item.
Note: The referring physician name and Unique Physician Identification (UPIN) Number must be reported for group 6 (procedure code 66985, 66986) and group 8 (procedure codes 66983 and 66984) facility services.
Payment for Terminated Procedures
An ASC claim for payment of terminated surgery must be accompanied by an operative report that specifies the following:
· Reason for termination of surgery;
· Services actually performed;
· Supplies actually provided;
· Services not performed that would have been performed if surgery had not been terminated;
· Supplies not provided that would have been provided if the surgery had not been terminated;
· Time actually spent in each stage, e.g., pre-operative, operative, and post-operative;
· Time that would have been spent in each of these stages if the surgery had not been terminated; and
· CPT-4 code for procedure had the surgery been performed.
Peer Review Organization (PRO) Prior Authorization
Assistant-at-cataract surgery for procedures 66852, 66920, 66940, requires a PRO prior authorization number.
There are 540 DRGs (Diagnosis Related Group) in the DRG Table.
drgtable
The Help button provides additional information on DRG pricing.
Diagnosis Related Groups (DRG)
Under the current prospective payment system, CMS pays for inpatient hospital services on the basis of a rate per discharge that varies by the DRG to which a beneficiary’s stay is assigned. The formula used to calculate payment for a specific case takes an individual hospital’s payment rate per case and multiplies it by the weight of the DRG to which the case is assigned. Each DRG weight represents the average resources required to care for cases in that particular DRG relative to the average resources used to treat cases in all DRGs.
Cases are classified into DRGs for payment under the prospective payment system based on the principal diagnosis, up to eight additional diagnoses, and up to six procedures performed during the stay, as well as age, sex, and discharge status of the patient.
Table Definitions
DRG Diagnosis Related Group
MDC Major Diagnostic Category
Indicator (*) Medicare Data have been supplemented by Data from 19 Sates for low volume DRGs
GMLOS Geometric Mean Length of Stay
AMLOS Arithmetic Mean Length of Stay
Relative Weights
DRG Payment
National Medicare Base Rate =$4,400 (Default)
DRGS 469 AND 470 contain cases which could not be assigned to valid DRGS
GEOMETRIC MEAN IS USED ONLY TO DETERMINE PAYMENT FOR TRANSFER CASES.
ARITHMETIC MEAN IS PRESENTED FOR INFORMATIONAL PURPOSES ONLY.
RELATIVE WEIGHTS ARE BASED ON MEDICARE PATIENT DATA AND MAY NOT BE APPROPRIATE FOR OTHER PATIENTS.
This software application calculates DRG payments based on the formula:
DRG Relative Weight x Hospital Base Rate = Hospital Payment
A national (default) hospital base rate of $4,400 is used to calculate national base rates. You may enter any user defined value from 1 to 99,999.
A MDC of “PRE” indicates a DRG case that is directly assigned based upon procedure codes.
Although RBRVS is the most widely used RVS (Relative Value Scale) it does not provide fee information for procedures and services not paid by Medicare. This results in “gaps” in medical fee schedules. Private payers including managed care who adopt RBRVS methodology are forced to price their gap claims on an individual basis or use alternative non RVS methodologies. Some simply pay out the claim while other defer to a review panel, bypassing the regular adjudication. This slows down the claims review process and often results in disputes and appeals with payers.
RBRVS EZ-Fees Gap Codes are provided under a license agreement with Relative Value Studies, Inc. (RVSI) publishers of the Complete RBRVS. We have selected RVSI’s Gap solution based on their reputation and experience in developing accurate, user-friendly coding and reimbursement guidelines for health care providers, consultants, and payers.
Integration of Gap Codes into RBRVS EZ-Fees is seamless. Simply enter your Gap license number under (Help-Upgrades-Gap License) and all Gap codes will appear on the main screen with a status indicator “g”. Since Gaps codes were designed for the RBRVS formula using the same CF (Conversion Factor) and GPCIs (Geographic Practice Cost Indicators) there is no math nor adjustments.
All versions of RBRVS EZ-Fees are upgradeable to include Gap Codes.
Gap Code List for 2022:
0001U, 0002M, 0002U, 0003M, 0003U, 0004M, 0005U, 0006M, 0007M, 0007U, 0008U, 0009U, 0010U, 0011M, 0011U, 0012M, 0012U, 0013M, 0013U, 0014M, 0014U, 0015M, 0016M, 0016U, 0017M, 0017U, 0018U, 0019U, 0021U, 0022U, 0023U, 0024U, 0025U, 0026U, 0027U, 0029U, 0030U, 0031U, 0032U, 0033U, 0034U, 0035U, 0036U, 0037U, 0038U, 0039U, 0040U, 0041U, 0042U, 0043U, 0044U, 0045U, 0046U, 0047U, 0048U, 0049U, 0050U, 0051U, 0052U, 0053U, 0054U, 0055U, 0056U, 0058U, 0059U, 0060U, 0061U, 0062U, 0063U, 0064U, 0065U, 0066U, 0067U, 0068U, 0069U, 0070U, 0071U, 0072U, 0073U, 0074U, 0075U, 0076U, 0077U, 0078U, 0080U, 0082U, 0083U, 0084U, 0086U, 0087U, 0088U, 0089U, 0090U, 0092U, 0093U, 0094U, 0095U, 0096U, 0097U, 0101U, 0102U, 0103U, 0105U, 0106U, 0107U, 0108U, 0109U, 0110U, 0111U, 0112U, 0113U, 0114U, 0115U, 0116U, 0117U, 0118U, 0119U, 0120U, 0121U, 0122U, 0123U, 0129U, 0130U, 0131U, 0132U, 0133U, 0134U, 0135U, 0136U, 0137U, 0138U, 0140U, 0141U, 0142U, 0143U, 0144U, 0145U, 0146U, 0147U, 0148U, 0149U, 0150U, 0151U, 0152U, 0153U, 0154U, 0155U, 0156U, 0157U, 0158U, 0159U, 0160U, 0161U, 0162U, 0163U, 0164U, 0165U, 0166U, 0167U, 0169U, 0170U, 0171U, 0172U, 0173U, 0174T, 0174U, 0175T, 0175U, 0176U, 0177U, 0178U, 0179U, 0180U, 0181U, 0182U, 0183U, 0184U, 0185U, 0186U, 0187U, 0188U, 0189U, 0190U, 0191U, 0192U, 0193U, 0194U, 0195U, 0196U, 0197U, 0198U, 0199U, 0200U, 0201U, 0202U, 0203U, 0204U, 0205U, 0206U, 0207U, 0209U, 0210U, 0211U, 0212U, 0213U, 0214U, 0215U, 0216U, 0217U, 0218U, 0219U, 0220U, 0221U, 0222U, 0223U, 0225U, 0227U, 0229U, 0230U, 0231U, 0232U, 0233U, 0234U, 0235U, 0236U, 0237U, 0238U, 0239U, 0240U, 0241U, 0242U, 0243U, 0244U, 0246U, 0247U, 0250U, 0251U, 0258U, 0259U, 0261U, 0263U, 0275U, 0279U, 0280U, 0281U, 0282U, 0283U, 0284U, 15824, 15825, 15826, 15828, 15829, 15847, 15876, 15877, 15878, 15879, 17380, 21088, 21742, 21743, 24940, 32850, 32855, 32856, 33929, 33930, 33933, 33940, 33944, 34839, 36415, 36416, 36468, 37195, 41820, 41821, 41850, 41870, 43496, 43647, 43648, 43881, 43882, 44132, 44133, 44135, 44136, 44137, 44715, 47133, 47143, 47144, 47145, 48550, 48551, 49906, 50300, 50323, 50325, 58974, 63043, 63044, 65760, 65765, 65767, 65771, 66983, 69090, 69710, 70170 TC, 70555 TC, 70557 TC, 70558 TC, 70559 TC, 74190 TC, 74235 TC, 74300 TC, 74301 TC, 74328 TC, 74329 TC, 74330 TC, 74340 TC, 74355 TC, 74360 TC, 74363 TC, 74445 TC, 74450 TC, 74470 TC, 74742 TC, 74775 TC, 75801 TC, 75803 TC, 75805 TC, 75807 TC, 75810 TC, 75894 TC, 75898 TC, 75956 TC, 75957 TC, 75958 TC, 75959 TC, 75970 TC, 76125 TC, 76140, 76932 TC, 76940 TC, 76941 TC, 76945 TC, 76975 TC, 76998 TC, 77013 TC, 77022TC, 77371, 77385, 77386, 77387, 77402, 77407, 77412, 77423, 77424, 77425, 78267, 78268, 78282 TC, 78414 TC, 78429 TC, 78430 TC, 78431 TC, 78432 TC, 78433 TC, 78434 TC, 78459 TC, 78491 TC, 78492 TC, 78608 TC, 78609 TC, 78811 TC, 78812 TC, 78813 TC, 78814 TC, 78815 TC, 78816TC, 79300TC, 79445TC, 80047, 80048, 80050, 80051, 80053, 80055, 80061, 80069, 80074, 80076, 80081, 80143, 80145, 80150, 80151, 80155, 80156, 80157, 80158, 80159, 80161, 80162, 80163, 80164, 80165, 80167, 80168, 80169, 80170, 80171, 80173, 80175, 80176, 80177, 80178, 80179, 80180, 80181, 80183, 80184, 80185, 80186, 80187, 80188, 80189, 80190, 80192, 80193, 80194, 80195, 80197, 80198, 80199, 80200, 80201, 80202, 80203, 80204, 80210, 80220, 80230, 80235, 80280, 80285, 80299, 80305, 80306, 80307, 80400, 80402, 80406, 80408, 80410, 80412, 80414, 80415, 80416, 80417, 80418, 80420, 80422, 80424, 80426, 80428, 80430, 80432, 80434, 80435, 80436, 80438, 80439, 81000, 81001, 81002, 81003, 81005, 81007, 81015, 81020, 81025, 81050, 81105, 81106, 81107, 81108, 81109, 81110, 81111, 81112, 81120, 81121, 81161, 81162, 81163, 81164, 81165, 81166, 81167, 81168, 81170, 81171, 81172, 81173, 81174, 81175, 81176, 81177, 81178, 81179, 81180, 81181, 81182, 81183, 81184, 81185, 81186, 81187, 81188, 81189, 81190, 81191, 81192, 81193, 81194, 81200, 81201, 81202, 81203, 81204, 81205, 81206, 81207, 81208, 81209, 81210, 81212, 81215, 81216, 81217, 81218, 81219, 81220, 81221, 81222, 81223, 81224, 81225, 81226, 81227, 81228, 81229, 81230, 81231, 81232, 81233, 81234, 81235, 81236, 81237, 81238, 81239, 81240, 81241, 81242, 81243, 81244, 81245, 81246, 81247, 81248, 81249, 81250, 81251, 81252, 81253, 81254, 81255, 81256, 81257, 81258, 81259, 81260, 81261, 81262, 81263, 81264, 81265, 81266, 81267, 81268, 81269, 81270, 81271, 81272, 81273, 81274, 81275, 81276, 81277, 81278, 81279, 81283, 81284, 81285, 81286, 81287, 81288, 81289, 81290, 81291, 81292, 81293, 81294, 81295, 81296, 81297, 81298, 81299, 81300, 81301, 81302, 81303, 81304, 81305, 81306, 81307, 81308, 81309, 81310, 81311, 81312, 81313, 81314, 81315, 81316, 81317, 81318, 81319, 81320, 81321, 81322, 81323, 81324, 81325, 81326, 81327, 81328, 81329, 81330, 81331, 81332, 81333, 81334, 81335, 81336, 81337, 81338, 81339, 81340, 81341, 81342, 81343, 81344, 81345, 81346, 81347, 81348, 81350, 81351, 81352, 81353, 81355, 81357, 81360, 81361, 81362, 81363, 81364, 81370, 81371, 81372, 81373, 81374, 81375, 81376, 81377, 81378, 81379, 81380, 81381, 81382, 81383, 81400, 81401, 81402, 81403, 81404, 81405, 81406, 81407, 81408, 81410, 81411, 81412, 81413, 81414, 81415, 81416, 81417, 81419, 81420, 81422, 81425, 81426, 81427, 81430, 81431, 81432, 81433, 81434, 81435, 81436, 81437, 81438, 81439, 81440, 81442, 81443, 81445, 81448, 81450, 81455, 81460, 81465, 81470, 81471, 81490, 81493, 81500, 81503, 81504, 81506, 81507, 81508, 81509, 81510, 81511, 81512, 81513, 81514, 81518, 81519, 81520, 81521, 81522, 81523, 81525, 81528, 81529, 81535, 81536, 81538, 81539, 81540, 81541, 81542, 81546, 81551, 81552, 81554, 81595, 81596, 82009, 82010, 82013, 82016, 82017, 82024, 82030, 82040, 82042, 82043, 82044, 82045, 82075, 82077, 82085, 82088, 82103, 82104, 82105, 82106, 82107, 82108, 82120, 82127, 82128, 82131, 82135, 82136, 82139, 82140, 82143, 82150, 82154, 82157, 82160, 82163, 82164, 82172, 82175, 82180, 82190, 82232, 82239, 82240, 82247, 82248, 82252, 82261, 82270, 82271, 82272, 82274, 82286, 82300, 82306, 82308, 82310, 82330, 82331, 82340, 82355, 82360, 82365, 82370, 82373, 82374, 82375, 82376, 82378, 82379, 82380, 82382, 82383, 82384, 82387, 82390, 82397, 82415, 82435, 82436, 82438, 82441, 82465, 82480, 82482, 82485, 82495, 82507, 82523, 82525, 82528, 82530, 82533, 82540, 82542, 82550, 82552, 82553, 82554, 82565, 82570, 82575, 82585, 82595, 82600, 82607, 82608, 82610, 82615, 82626, 82627, 82633, 82634, 82638, 82642, 82652, 82653, 82656, 82657, 82658, 82664, 82668, 82670, 82671, 82672, 82677, 82679, 82681, 82693, 82696, 82705, 82710, 82715, 82725, 82726, 82728, 82731, 82735, 82746, 82747, 82757, 82759, 82760, 82775, 82776, 82777, 82784, 82785, 82787, 82800, 82803, 82805, 82810, 82820, 82930, 82938, 82941, 82943, 82945, 82946, 82947, 82948, 82950, 82951, 82952, 82955, 82960, 82962, 82963, 82965, 82977, 82978, 82979, 82985, 83001, 83002, 83003, 83006, 83009, 83010, 83012, 83013, 83014, 83015, 83018, 83020, 83021, 83026, 83030, 83033, 83036, 83037, 83045, 83050, 83051, 83060, 83065, 83068, 83069, 83070, 83080, 83088, 83090, 83150, 83491, 83497, 83498, 83500, 83505, 83516, 83518, 83519, 83520, 83521, 83525, 83527, 83528, 83529, 83540, 83550, 83570, 83582, 83586, 83593, 83605, 83615, 83625, 83630, 83631, 83632, 83633, 83655, 83661, 83662, 83663, 83664, 83670, 83690, 83695, 83698, 83700, 83701, 83704, 83718, 83719, 83721, 83722, 83727, 83735, 83775, 83785, 83789, 83825, 83835, 83857, 83861, 83864, 83872, 83873, 83874, 83876, 83880, 83883, 83885, 83915, 83916, 83918, 83919, 83921, 83930, 83935, 83937, 83945, 83950, 83951, 83970, 83986, 83987, 83992, 83993, 84030, 84035, 84060, 84066, 84075, 84078, 84080, 84081, 84085, 84087, 84100, 84105, 84106, 84110, 84112, 84119, 84120, 84126, 84132, 84133, 84134, 84135, 84138, 84140, 84143, 84144, 84145, 84146, 84150, 84152, 84153, 84154, 84155, 84156, 84157, 84160, 84163, 84165, 84166, 84181, 84182, 84202, 84203, 84206, 84207, 84210, 84220, 84228, 84233, 84234, 84235, 84238, 84244, 84252, 84255, 84260, 84270, 84275, 84285, 84295, 84300, 84302, 84305, 84307, 84311, 84315, 84375, 84376, 84377, 84378, 84379, 84392, 84402, 84403, 84410, 84425, 84430, 84431, 84432, 84436, 84437, 84439, 84442, 84443, 84445, 84446, 84449, 84450, 84460, 84466, 84478, 84479, 84480, 84481, 84482, 84484, 84485, 84488, 84490, 84510, 84512, 84520, 84525, 84540, 84545, 84550, 84560, 84577, 84578, 84580, 84583, 84585, 84586, 84588, 84590, 84591, 84597, 84600, 84620, 84630, 84681, 84702, 84703, 84704, 84830, 85002, 85004, 85007, 85008, 85009, 85013, 85014, 85018, 85025, 85027, 85032, 85041, 85044, 85045, 85046, 85048, 85049, 85055, 85130, 85170, 85175, 85210, 85220, 85230, 85240, 85244, 85245, 85246, 85247, 85250, 85260, 85270, 85280, 85290, 85291, 85292, 85293, 85300, 85301, 85302, 85303, 85305, 85306, 85307, 85335, 85337, 85345, 85347, 85348, 85360, 85362, 85366, 85370, 85378, 85379, 85380, 85384, 85385, 85390, 85397, 85400, 85410, 85415, 85420, 85421, 85441, 85445, 85460, 85461, 85475, 85520, 85525, 85530, 85536, 85540, 85547, 85549, 85555, 85557, 85576, 85597, 85598, 85610, 85611, 85612, 85613, 85635, 85651, 85652, 85660, 85670, 85675, 85705, 85730, 85732, 85810, 86000, 86001, 86003, 86005, 86008, 86015, 86021, 86022, 86023, 86036, 86037, 86038, 86039, 86051, 86052, 86053, 86060, 86063, 86140, 86141, 86146, 86147, 86148, 86152, 86155, 86156, 86157, 86160, 86161, 86162, 86171, 86200, 86215, 86225, 86226, 86231, 86235, 86255, 86256, 86258, 86277, 86280, 86294, 86300, 86301, 86304, 86305, 86308, 86309, 86310, 86316, 86317, 86318, 86320, 86325, 86327, 86328, 86329, 86331, 86332, 86334, 86335, 86336, 86337, 86340, 86341, 86343, 86344, 86352, 86353, 86355, 86356, 86357, 86359, 86360, 86361, 86362, 86363, 86364, 86367, 86376, 86381, 86382, 86384, 86386, 86403, 86406, 86430, 86431, 86480, 86481, 86485, 86590, 86592, 86593, 86596, 86602, 86603, 86606, 86609, 86611, 86612, 86615, 86617, 86618, 86619, 86622, 86625, 86628, 86631, 86632, 86635, 86638, 86641, 86644, 86645, 86648, 86651, 86652, 86653, 86654, 86658, 86663, 86664, 86665, 86666, 86668, 86671, 86674, 86677, 86682, 86684, 86687, 86688, 86689, 86692, 86694, 86695, 86696, 86698, 86701, 86702, 86703, 86704, 86705, 86706, 86707, 86708, 86709, 86710, 86711, 86713, 86717, 86720, 86723, 86727, 86732, 86735, 86738, 86741, 86744, 86747, 86750, 86753, 86756, 86757, 86759, 86762, 86765, 86768, 86769, 86771, 86774, 86777, 86778, 86780, 86784, 86787, 86788, 86789, 86790, 86793, 86794, 86800, 86803, 86804, 86805, 86806, 86807, 86808, 86812, 86813, 86816, 86817, 86821, 86825, 86826, 86828, 86829, 86830, 86831, 86832, 86833, 86834, 86835, 86850, 86860, 86870, 86880, 86885, 86886, 86890, 86891, 86900, 86901, 86902, 86904, 86905, 86906, 86910, 86911, 86920, 86921, 86922, 86923, 86927, 86930, 86931, 86932, 86940, 86941, 86945, 86950, 86960, 86965, 86970, 86971, 86972, 86975, 86976, 86977, 86978, 86985, 87003, 87015, 87040, 87045, 87046, 87070, 87071, 87073, 87075, 87076, 87077, 87081, 87084, 87086, 87088, 87101, 87102, 87103, 87106, 87107, 87109, 87110, 87116, 87118, 87140, 87143, 87147, 87149, 87150, 87152, 87153, 87154, 87158, 87164, 87166, 87168, 87169, 87172, 87176, 87177, 87181, 87184, 87185, 87186, 87187, 87188, 87190, 87197, 87205, 87206, 87207, 87209, 87210, 87220, 87230, 87250, 87252, 87253, 87254, 87255, 87260, 87265, 87267, 87269, 87270, 87271, 87272, 87273, 87274, 87275, 87276, 87278, 87279, 87280, 87281, 87283, 87285, 87290, 87299, 87300, 87301, 87305, 87320, 87324, 87327, 87328, 87329, 87332, 87335, 87336, 87337, 87338, 87339, 87340, 87341, 87350, 87380, 87385, 87389, 87390, 87391, 87400, 87420, 87425, 87427, 87428, 87430, 87449, 87451, 87471, 87472, 87475, 87476, 87480, 87481, 87482, 87483, 87485, 87486, 87487, 87490, 87491, 87492, 87493, 87495, 87496, 87497, 87498, 87500, 87501, 87502, 87503, 87505, 87506, 87507, 87510, 87511, 87512, 87516, 87517, 87520, 87521, 87522, 87525, 87526, 87527, 87528, 87529, 87530, 87531, 87532, 87533, 87534, 87535, 87536, 87537, 87538, 87539, 87540, 87541, 87542, 87550, 87551, 87552, 87555, 87556, 87557, 87560, 87561, 87562, 87563, 87580, 87581, 87582, 87590, 87591, 87592, 87623, 87624, 87625, 87631, 87632, 87633, 87634, 87635, 87636, 87637, 87640, 87641, 87650, 87651, 87652, 87653, 87660, 87661, 87662, 87797, 87798, 87799, 87800, 87801, 87802, 87803, 87804, 87806, 87807, 87808, 87809, 87810, 87850, 87880, 87899, 87900, 87901, 87902, 87903, 87904, 87905, 87906, 87910, 87912, 88000, 88005, 88007, 88012, 88014, 88016, 88020, 88025, 88027, 88028, 88029, 88036, 88037, 88040, 88130, 88140, 88142, 88143, 88147, 88148, 88150, 88152, 88153, 88155, 88164, 88165, 88166, 88167, 88174, 88175, 88230, 88233, 88235, 88237, 88239, 88240, 88241, 88245, 88248, 88249, 88261, 88262, 88263, 88264, 88267, 88269, 88271, 88272, 88273, 88274, 88275, 88280, 88283, 88285, 88289, 88371, 88372, 88720, 88738, 88740, 88741, 89050, 89051, 89055, 89060, 89125, 89160, 89190, 89250, 89300, 89310, 89320, 89321, 89322, 89325, 89329, 89330, 89331, 90281, 90283, 90284, 90287, 90288, 90291, 90296, 90371, 90375, 90376, 90378, 90384, 90385, 90386, 90389, 90393, 90396, 90399, 90476, 90477, 90581, 90585, 90586, 90632, 90633, 90634, 90636, 90647, 90648, 90649, 90650, 90653, 90654, 90655, 90656, 90657, 90658, 90660, 90661, 90662, 90664, 90666, 90667, 90668, 90670, 90672, 90673, 90675, 90676, 90680, 90685, 90686, 90687, 90688, 90690, 90691, 90696, 90698, 90700, 90702, 90707, 90710, 90713, 90714, 90715, 90716, 90717, 90723, 90732, 90733, 90734, 90736, 90738, 90739, 90740, 90743, 90744, 90746, 90747, 90748, 90749, 90867, 90868, 90869, 90882, 90889, 90952, 90953, 90989, 90993, 92531, 92532, 92533, 92534, 92590, 92591, 92592, 92593, 92594, 92595, 92921, 92925, 92929, 92934, 92938, 92944, 92978 TC, 92979 TC, 93315 TC, 93317 TC, 93318 TC, 93571 TC, 93572 TC, 93600 TC, 93602 TC, 93603 TC, 93609 TC, 93610 TC, 93612 TC, 93615 TC, 93616 TC, 93618 TC, 93619 TC, 93620 TC, 93621 TC, 93622 TC, 93623 TC, 93624 TC, 93631 TC, 93640 TC, 93641 TC, 93662TC, 94642, 95120, 95125, 95130, 95131, 95132, 95133, 95134, 95824 TC, 95941, 95965 TC, 95966 TC, 95967TC, 96020, 96020TC, 96376, 97039, 97139, 97169, 97170, 97171, 97172, 97545, 97546, 97602, 99000, 99001, 99002, 99026, 99027, 99050, 99056, 99058, 99075, 99100, 99116, 99135, 99140, 99172, 99190, 99191, 99192, 99288, 99450, 99455, 99456, 99500, 99501, 99502, 99503, 99504, 99505, 99506, 99507, 99509, 99510, 99511, 99512, 99601, 99602, 99605, 99606, 99607, A0225, G0008, G0009, G0010, G0027, G0103, G0103 26, G0103 TC, G0123, G0129, G0143, G0144, G0145, G0147, G0148, G0151, G0152, G0153, G0155, G0156, G0157, G0158, G0159, G0160, G0161, G0162, G0175, G0176, G0177, G0186, G0219, G0219 26, G0219 TC, G0252 TC, G0259, G0260, G0269, G0282, G0306, G0307, G0328, G0378, G0379, G0380, G0381, G0382, G0383, G0384, G0410, G0411, G0428, G0432, G0448, G0460, G0471, G0472, G2211, P2031, P2038, P3000, P7001, P9612, P9615, Q0111, Q0112, Q0113, Q0114, Q0115, Q3014, Q4001, Q4002, Q4003, Q4004, Q4005, Q4006, Q4007, Q4008, Q4009, Q4010, Q4011, Q4012, Q4013, Q4014, Q4015, Q4016, Q4017, Q4018, Q4019, Q4020, Q4021, Q4022, Q4023, Q4024, Q4025, Q4026, Q4027, Q4028, Q4029, Q4030, Q4031, Q4032, Q4033, Q4034, Q4035, Q4036, Q4037, Q4038, Q4039, Q4040, Q4041, Q4042, Q4043, Q4044, Q4045, Q4046, Q4047, Q4048, Q4049, Q4050, Q4051, R0070, R0075, S0601, S0610, S0612, S0620, S0621, S0800, S0810, S2205, S2206, S2207, S2208, S2209, S2300, S2340, S2350, S2351, S3652, S9090
CPT® Codes and Descriptions © 2021 AMA All Rights Reserved CPT® is a registered trademark of the American Medical Association.
Carrier and Zip Code Tables
Used by developers for advanced RBRVS fee analysis
Export to Access or CSV
Updated every year
RBRVS EZ-Fees Pro Plus exports two tables related to zip codes, carriers and localities
GPCI Locality Table State, County, Carrier and Locality.
| State | ST | DESC | county | carrier | loccode | work | pract | malp |
|---|---|---|---|---|---|---|---|---|
| ALABAMA | AL | ALABAMA | ALL COUNTIES | 00510 | 00 | 1 | 0.847 | 0.74 |
| ALASKA | AK | ALASKA | ALL COUNTIES | 00831 | 01 | 1.017 | 1.105 | 1.013 |
| ARIZONA | AZ | ARIZONA | ALL COUNTIES | 03102 | 00 | 1 | 0.994 | 1.052 |
| ARKANSAS | AR | ARKANSAS | ALL COUNTIES | 00520 | 13 | 1 | 0.832 | 0.431 |
| CALIFORNIA | CA | REST OF CALIFORNIA* | ALL OTHER COUNTIES | 31146 | 99 | 1.007 | 1.054 | 0.721 |
| CALIFORNIA | CA | VENTURA, CA | VENTURA | 31146 | 17 | 1.028 | 1.181 | 0.732 |
| CALIFORNIA | CA | LOS ANGELES, CA | LOS ANGELES | 31146 | 18 | 1.041 | 1.158 | 0.939 |
| CALIFORNIA | CA | ANAHEIM/SANTA ANA, CA | ORANGE | 31146 | 26 | 1.034 | 1.238 | 0.939 |
| CALIFORNIA | CA | REST OF CALIFORNIA* | ALL OTHER COUNTIES | 31140 | 99 | 1.007 | 1.054 | 0.721 |
| CALIFORNIA | CA | MARIN/NAPA/SOLANO, CA | MARIN, NAPA, AND SOLANO | 31140 | 03 | 1.035 | 1.342 | 0.64 |
| CALIFORNIA | CA | SAN FRANCISCO, CA | SAN FRANCISCO | 31140 | 05 | 1.06 | 1.546 | 0.64 |
| CALIFORNIA | CA | SAN MATEO, CA | SAN MATEO | 31140 | 06 | 1.073 | 1.539 | 0.629 |
| CALIFORNIA | CA | SANTA CLARA, CA | SANTA CLARA | 31140 | 09 | 1.083 | 1.543 | 0.595 |
| CALIFORNIA | CA | OAKLAND/BERKLEY, CA | ALMEDA AND CONTRA COSTA | 31140 | 07 | 1.054 | 1.373 | 0.64 |
| COLORADO | CO | COLORADO | ALL COUNTIES | 00824 | 01 | 1 | 1.015 | 0.79 |
| CONNECTICUT | CT | CONNECTICUT | ALL COUNTIES | 00591 | 00 | 1.038 | 1.172 | 0.886 |
| DELAWARE | DE | DELAWARE | ALL COUNTIES | 00902 | 01 | 1.012 | 1.02 | 0.877 |
| DISTRICT OF COLUMBIA | DC | DC + MD/VA SUBURBS | DISTRICT OF COLUMBIA; ALEXANDRIA CITY, ARLINGTON, FAIRFAX, FAIRFAX CITY, FALLS CHURCH CITY IN VIRGINIA; MONTGOMERY AND PRINCE GEORGE’S IN MARYLAND | 00903 | 01 | 1.048 | 1.252 | 0.911 |
| FLORIDA | FL | MIAMI, FL | DADE AND MONROE | 00590 | 04 | 1 | 1.048 | 2.233 |
| FLORIDA | FL | FORT LAUDERDALE, FL | BROWARD, COLLIER, INDIAN RIVER, LEE, MARTIN, PALM BEACH, AND ST. LUCIE | 00590 | 03 | 1 | 0.99 | 1.675 |
| FLORIDA | FL | REST OF FLORIDA | ALL OTHER COUNTIES | 00590 | 99 | 1 | 0.936 | 1.251 |
| GEORGIA | GA | REST OF GEORGIA | ALL OTHER COUNTIES | 00511 | 99 | 1 | 0.874 | 0.95 |
| GEORGIA | GA | ATLANTA, GA | BUTTS, CHEROKEE, CLAYTON, COBB, DEKALB, DOUGLAS, FAYETTE, FORSYTH, FULTON, GWINNETT, HENRY, NEWTON, PAULDING, ROCKDALE AND WALTON | 00511 | 01 | 1.01 | 1.091 | 0.95 |
| NEW YORK | NY | QUEENS, NY | QUEENS | 14330 | 04 | 1.032 | 1.23 | 1.682 |
| NEW YORK | NY | REST OF NEW YORK | ALL OTHER COUNTIES | 00801 | 99 | 1 | 0.919 | 0.666 |
| NEW YORK | NY | NYC SUBURBS/LONG I., NY | BRONX, KINGS, NASSAU, RICHMOND, ROCKLAND, SUFFOLK AND WESTCHESTER | 00803 | 02 | 1.052 | 1.283 | 1.756 |
| NEW YORK | NY | MANHATTAN, NY | NEW YORK | 00803 | 01 | 1.065 | 1.3 | 1.48 |
| NORTH CAROLINA | NC | NORTH CAROLINA | ALL COUNTIES | 05535 | 00 | 1 | 0.922 | 0.63 |
| NORTH DAKOTA | ND | NORTH DAKOTA | ALL COUNTIES | 03302 | 01 | 1 | 0.861 | 0.593 |
| OHIO | OH | OHIO | ALL COUNTIES | 00883 | 00 | 1 | 0.934 | 0.96 |
| OKLAHOMA | OK | OKLAHOMA | ALL COUNTIES | 00522 | 00 | 1 | 0.856 | 0.376 |
| OREGON | OR | PORTLAND, OR | CLACKAMAS, MULTNOMAH AND WASHINGTON | 00835 | 01 | 1.002 | 1.059 | 0.434 |
| OREGON | OR | REST OF OREGON | ALL OTHER COUNTIES | 00835 | 99 | 1 | 0.927 | 0.434 |
| PENNSYLVANIA | PA | METROPOLITAN PHILADELPHIA, | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | 00865 | 01 | 1.016 | 1.106 | 1.364 |
| PENNSYLVANIA | PA | REST OF PENNSYLVANIA | ALL OTHER COUNTIES | 00865 | 99 | 1 | 0.904 | 0.793 |
| PUERTO RICO | PR | PUERTO RICO | ALL COUNTY EQUIVALENTS | 00973 | 20 | 1 | 0.699 | 0.257 |
| RHODE ISLAND | RI | RHODE ISLAND | ALL COUNTIES | 00524 | 01 | 1.045 | 0.991 | 0.895 |
| SOUTH CAROLINA | SC | SOUTH CAROLINA | ALL COUNTIES | 00880 | 01 | 1 | 0.894 | 0.388 |
| SOUTH DAKOTA | SD | SOUTH DAKOTA | ALL COUNTIES | 03402 | 02 | 1 | 0.877 | 0.359 |
| TENNESSEE | TN | TENNESSEE | ALL COUNTIES | 05440 | 35 | 1 | 0.881 | 0.621 |
| TEXAS | TX | BRAZORIA, TX | BRAZORIA | 00900 | 09 | 1.02 | 0.963 | 1.277 |
| TEXAS | TX | DALLAS, TX | DALLAS | 00900 | 11 | 1.009 | 1.064 | 1.044 |
| TEXAS | TX | GALVESTON, TX | GALVESTON | 00900 | 15 | 1 | 0.954 | 1.277 |
| TEXAS | TX | HOUSTON, TX | HARRIS | 00900 | 18 | 1.016 | 1.016 | 1.276 |
| TEXAS | TX | BEAUMONT, TX | JEFFERSON | 00900 | 20 | 1 | 0.862 | 1.277 |
| TEXAS | TX | FORT WORTH, TX | TARRANT | 00900 | 28 | 1 | 0.991 | 1.044 |
| TEXAS | TX | AUSTIN, TX | TRAVIS | 00900 | 31 | 1 | 1.048 | 0.97 |
| TEXAS | TX | REST OF TEXAS | ALL OTHER COUNTIES | 00900 | 99 | 1 | 0.866 | 1.12 |
Zip Code to Carrier Crosswalk
| Record Layout: |
| Field | Type | Size | Description |
| Zip Code | Text | 5 | 5 digit Zip Code |
| Carrier | Text | 5 | 5 digit number assigned to Part B carrier |
| Locality | Text | 2 | Two Digit Locality – “99” indicates statewide or rest of state |
| Rural Ind | Text | 1 | HPSA Bonus Area Designator – “R” for Rural |
| Version | Text | 5 | Year plus quarter – “20061” represents 2006 1st quarter |
| Work | Num | 9.999 | RBRVS Work component |
| Pract | Num | 9.999 | RBRVS Practice component (non facility) |
| Malp | Num | 9.999 | RBRVS Malpractice component |
| State | Text | 2 | Two letter abbreviation for state – “PA” for Pennsylvania |
| County | Text | 50 | Description of county or counties – “BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA” |
| Desc | Text | 50 | METROPOLITAN PHILADELPHIA |
Sample Data download sample zip code to carrier crosswalk file 500 records 10KB download
| ZIPCODE | CARRIER | LOCALITY | RURAL IND | VERSION | WORK | PRACT | MALP | STATE | COUNTY | DESC |
|---|---|---|---|---|---|---|---|---|---|---|
| 18847 | 00865 | 99 | R | 20061 | 1 | 0.902 | 0.806 | PA | ALL OTHER COUNTIES | REST OF PENNSYLVANIA |
| 18848 | 00865 | 99 | R | 20061 | 1 | 0.902 | 0.806 | PA | ALL OTHER COUNTIES | REST OF PENNSYLVANIA |
| 18850 | 00865 | 99 | R | 20061 | 1 | 0.902 | 0.806 | PA | ALL OTHER COUNTIES | REST OF PENNSYLVANIA |
| 18851 | 00865 | 99 | R | 20061 | 1 | 0.902 | 0.806 | PA | ALL OTHER COUNTIES | REST OF PENNSYLVANIA |
| 18853 | 00865 | 99 | R | 20061 | 1 | 0.902 | 0.806 | PA | ALL OTHER COUNTIES | REST OF PENNSYLVANIA |
| 18854 | 00865 | 99 | R | 20061 | 1 | 0.902 | 0.806 | PA | ALL OTHER COUNTIES | REST OF PENNSYLVANIA |
| 18901 | 00865 | 01 | 20061 | 1.016 | 1.104 | 1.386 | PA | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | METROPOLITAN PHILADELPHIA, | |
| 18910 | 00865 | 01 | 20061 | 1.016 | 1.104 | 1.386 | PA | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | METROPOLITAN PHILADELPHIA, | |
| 18911 | 00865 | 01 | 20061 | 1.016 | 1.104 | 1.386 | PA | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | METROPOLITAN PHILADELPHIA, | |
| 18912 | 00865 | 01 | 20061 | 1.016 | 1.104 | 1.386 | PA | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | METROPOLITAN PHILADELPHIA, | |
| 18913 | 00865 | 01 | 20061 | 1.016 | 1.104 | 1.386 | PA | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | METROPOLITAN PHILADELPHIA, | |
| 18914 | 00865 | 01 | 20061 | 1.016 | 1.104 | 1.386 | PA | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | METROPOLITAN PHILADELPHIA, | |
| 18915 | 00865 | 01 | 20061 | 1.016 | 1.104 | 1.386 | PA | BUCKS, CHESTER, DELAWARE, MONTGOMERY AND PHILADELPHIA | METROPOLITAN PHILADELPHIA, |
Notes: The main purpose of this table is to provide a crosswalk between zip code and Medicare locality. This table is used by software developers who want to write a routine that will allow the user to enter a zip code and return a value that contains the carrier number plus locality. For example zip code “18915” returns “00865 01”. This information can then be used to with the
RBRVS EZ-Fees® National Access® Table Export Wizard to look up specific Medicare reimbursement rates.

