Who Uses RBRVS EZ-Fees?
Providers
- Physicians and other healthcare professionals
Payers
- Insurance companies
- Federal health plans
- State Agencies
- Managed care
- (HMO, PPO, TPA, PHO, IPA)
Administrators
- Office managers
- Consultants
- Accountants
- Billing services
- 3rd Party Administrators
- CFOs, CEOs, and CPAs
Other Interested Parties
- Life care planners
- Actuaries
- Lawyers
- Medical societies
- State and Federal agencies
Introductory Video
RBRVS, or resource-based relative value scale, is a structured and scalable payment system used by CMS (Medicare/Medicaid), many state workers compensation boards, and nearly all HMO’s (health maintenance organizations). It is a fairly complicated system to navigate without help. RBRVS EZ-Fees is a low cost PC software application that simplifies RBRVS with one main screen and no complicated manuals or training. With a few clicks you can look up any medical fee for over 10,000 payment localities.
Note, Medicare does not pay for all CPT/HCPCS services by not assigning (RVUs) relative value units. Codes not valued by Medicare are referred to as gap codes. As an added value, RBRVS EZ-Fees offers an optional gap license.
Since 1998, RBRVS EZ-Fees has helped thousands of healthcare professionals simplify the Medicare payment formula.
With a few clicks you can create medical fee schedules without government downloads or complicated formulas. Most users have mastered our software in 5 minutes!

What are people saying about us?
If you’re not using the latest RVUs and CF you may be leaving money on the table.
No messy government downloads or complicated formulas. Let us keep you up-to-date with the #1 RBRVS solution on the market.


Take A Quick Tour
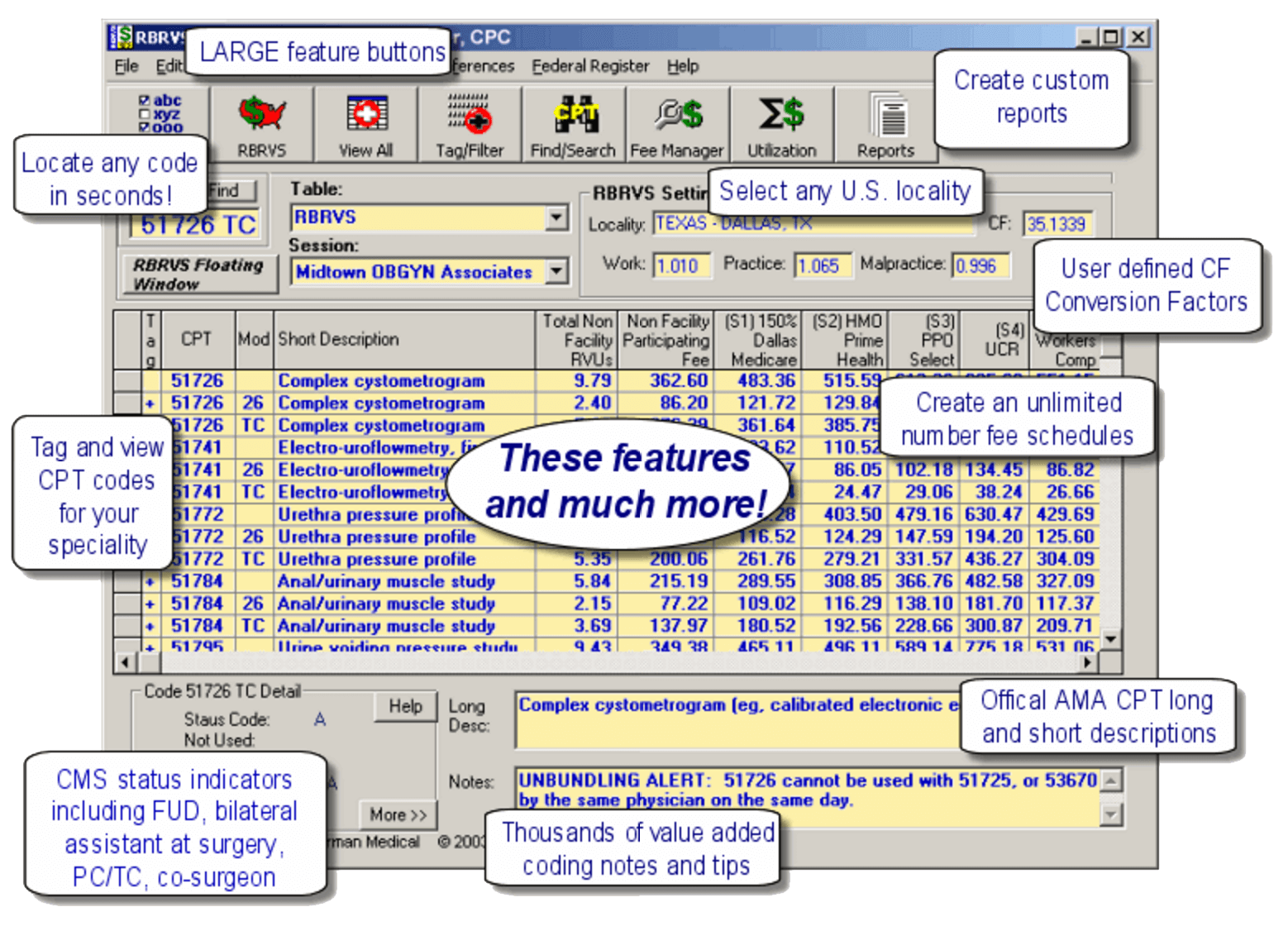


The red button of the U.S. allows the user to look up and select a Medicare locality. The Select by State tab allows lookups by state, city, county, Part B carrier, locality, and browse work, practice and malpractice GPCIs.
See second image for Select by Zip Code Tab


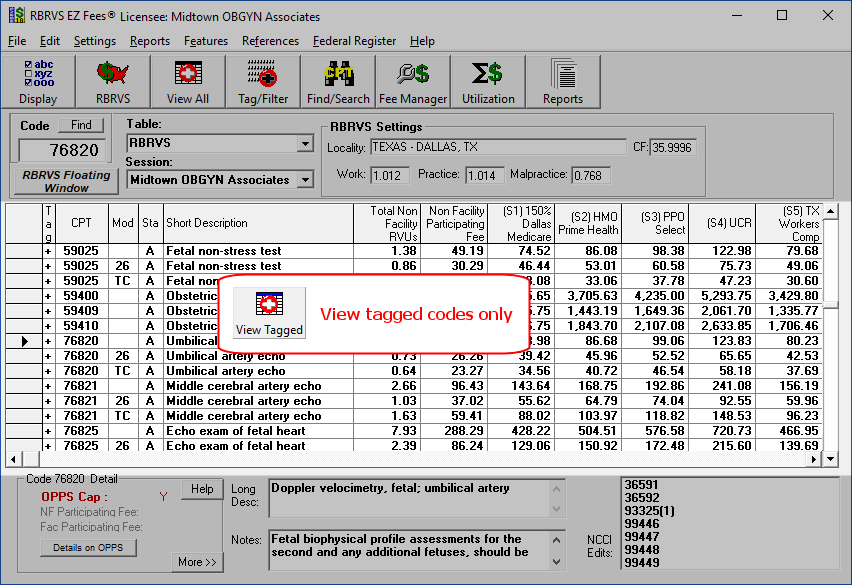
The View Tagged button allows for viewing tagged codes only. Tagging allows you to select only those code you are interested in viewing or printing. Tagged codes have a “+” sign on the main screen.

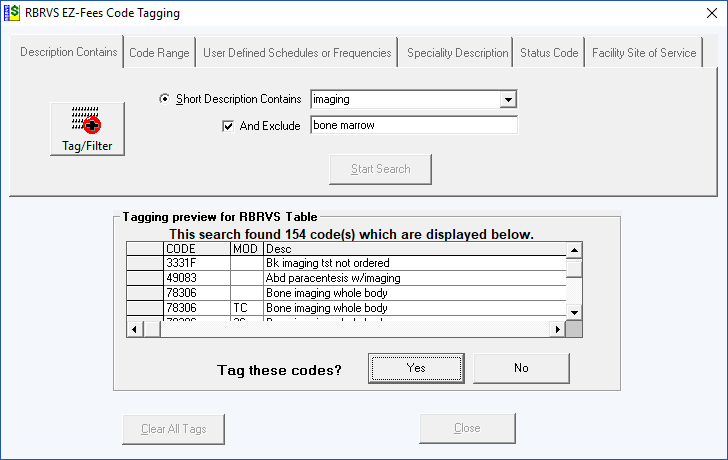
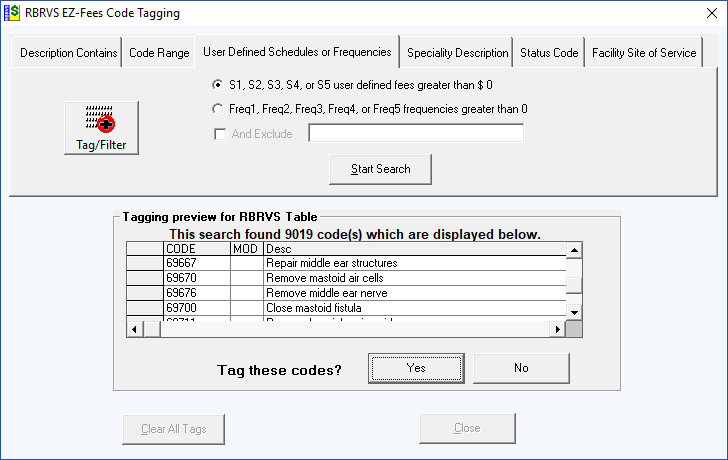
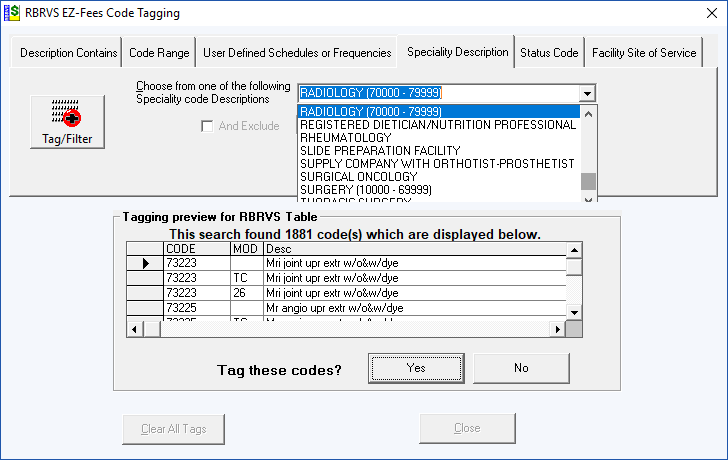
The Tag/Filter button allows for tagging (book marking) procedure codes based on Description, Code Range, Fee or Frequency Values, Medical Specialty and Code Status. Tagged codes can then be selected to be viewed only on the main screen and printed. Tagging is cumulative – meaning you can make several passes to tag additional codes that meet different search criteria. You can clear, save and load a tag list. RBRVS EZFees contains several tagging methods.



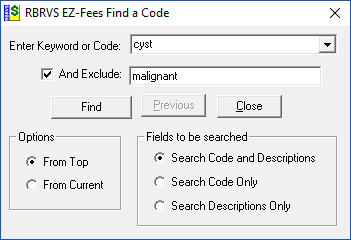
The Find / Search button searches for any keyword or code with several options to assist in locating difficult to find codes. The dropdown list hold the last 10 keywords.

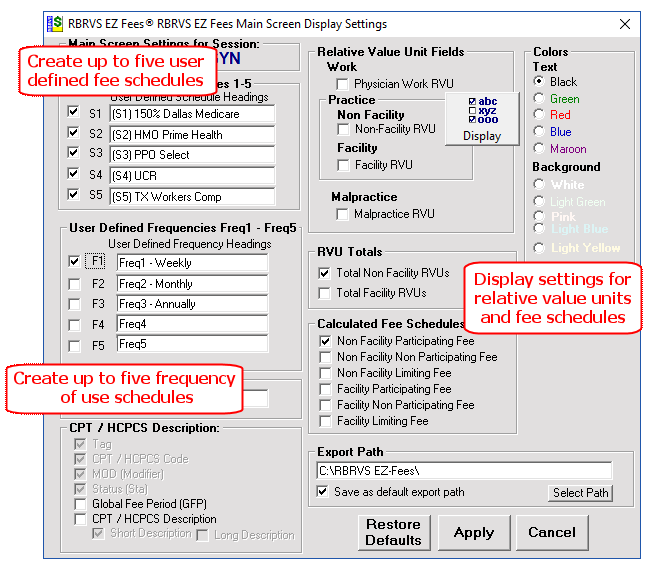
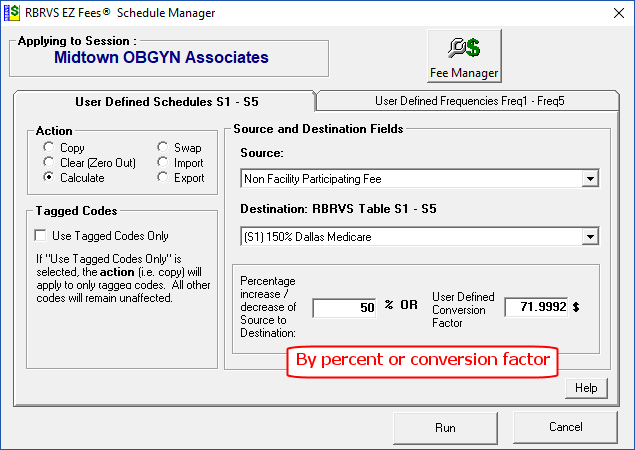
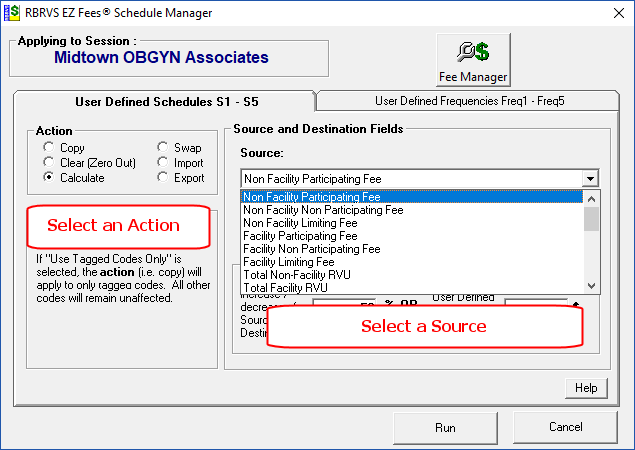
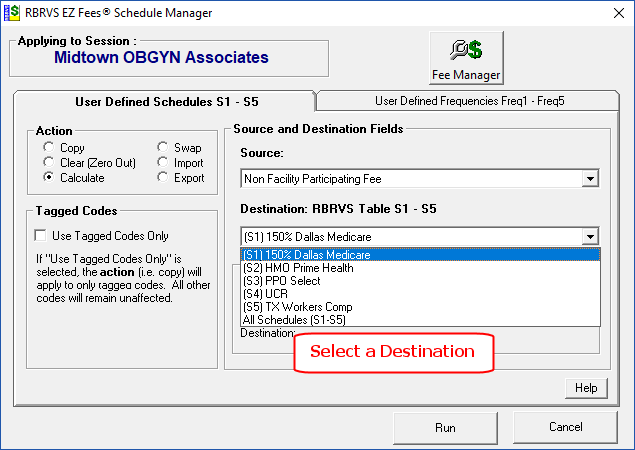
The Fee Manager button allows the user to create and modify fee schedules. In this example, the user is creating a fee schedule called Dallas Medicare that is above the Non participating Medicare Fee Schedule for Dallas, Texas.
The “Source” can be any of the 6 Medicare Fee Schedules or any of the 5 User Defined Fee Schedules.
The “Destination” is any of the 5 User defined Fee Schedules
There are two tabs in the Schedule Manager: Fee Schedules and Frequency Schedules. You can perform the same operations on up to 5 User Define Frequency Schedules.



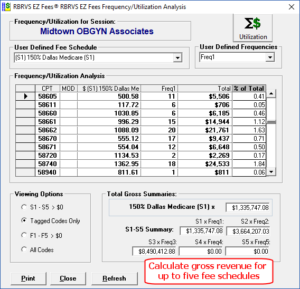
The Utilization / Frequency feature shows procedure code, selected user defined fee and frequency schedule and total (user defined fee time frequency and percent of total schedule).

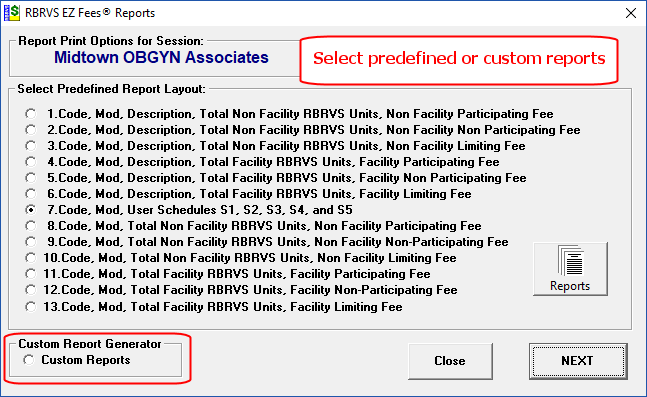
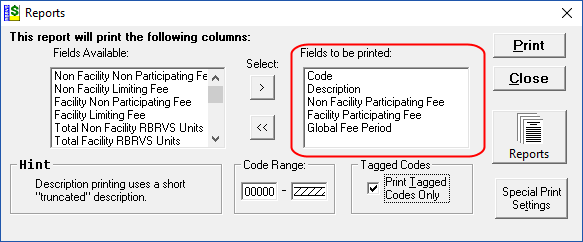
The Reports button brings up 13 common pre-defined report layouts.For custom reports select the “Custom Reports” option. Custom Reports allows for user defined fields. The “Print Tagged Codes Only” check box is an excellent way to print only those codes you wish to include in your report.




 Bob Shuman
Bob Shuman